
Why Does Therapy Not Work for Me? Unblock Healing
You leave a session thinking, “I can explain my childhood perfectly, so why do I still spiral in relationships?” You know your patterns. You can name them. You may even predict them before they happen. But your body still clenches when someone pulls away, you still shut down when conflict appears, or you still feel crushed by a text that sounds slightly off.
That gap is where so many people get discouraged. You’ve done the work. You’ve shown up. You’ve talked. And still, something hasn’t shifted.
If you’ve been asking why does therapy not work for me, I want to say this clearly. It often isn’t because you’re resistant, broken, or incapable of healing. Many people don’t improve in standard therapy, and some feel worse. ReachLink notes that 20-25% of therapy clients show no meaningful improvement, while 5-10% deteriorate post-treatment. That doesn’t mean therapy is useless. It means the fit, method, and relationship matter far more than is often communicated.
For people with insecure attachment, the problem is often not a lack of insight. It’s that insight alone doesn’t reach the place where the pattern lives.
That Familiar Feeling of Being Stuck in Therapy
You talk for fifty minutes. You describe the breakup, the overthinking, the shutdown after conflict, the way you keep choosing emotionally unavailable people. Your therapist nods, reflects, and maybe helps you connect it back to childhood. You leave with language for the pattern, but no relief from it.
That experience is more common than people think.
I often hear versions of the same story. “My therapist is nice, but I don’t feel different.” “I understand why I do this, but I still can’t stop.” “Every session feels intellectual, and then I fall apart the second I’m triggered in real life.” Sometimes the person starts blaming themselves. They assume they’re too complicated. Too self-aware. Too damaged. Too late.
That conclusion is usually wrong.
When effort doesn’t lead to change
Many clients who feel defeated by therapy are doing exactly what therapy asked of them. They show up consistently. They reflect thoroughly. They try to be honest. They read the books, journal between sessions, and practice coping tools. Yet their core reactions stay intact.
That doesn’t automatically mean they failed at therapy. It often means the therapy they received didn’t match what their system needed.
Practical rule: If you leave therapy with more understanding but not more capacity, something important may be missing.
For attachment wounds, the missing piece is often felt safety. A person may be able to think clearly in session while their body remains braced for rejection, engulfment, criticism, or abandonment. In that state, the old pattern doesn’t loosen. It rehearses itself.
What stuck often looks like
Being stuck in therapy can look like:
- Explaining instead of changing: You can describe your history in detail, but your reactions still feel automatic.
- Performing insight: You say the right things in session, then feel ashamed that your actual life still feels messy.
- Leaving dysregulated: Sessions open painful material but don’t help your body settle afterward.
- Repeating the same week: Different examples, same emotional loop.
Some people also start dreading appointments and can’t explain why. They may like the therapist and still feel unseen. They may talk easily and still feel emotionally alone in the room.
That’s not a small issue. It’s clinical information.
The better question
Instead of asking, “What’s wrong with me?” ask, “What kind of help does my nervous system respond to?”
That question opens the door to a different kind of healing. One that doesn’t ask you to think your way out of survival responses. One that respects that relationship patterns are not just beliefs. They are lived, embodied expectations.
When Talking Is Not Enough The Insight-Regulation Gap
Traditional talk therapy often starts from a reasonable assumption. If you understand your thoughts, beliefs, and patterns, you can begin to change them. Sometimes that works well.
But attachment wounds often don’t operate like a purely cognitive problem.
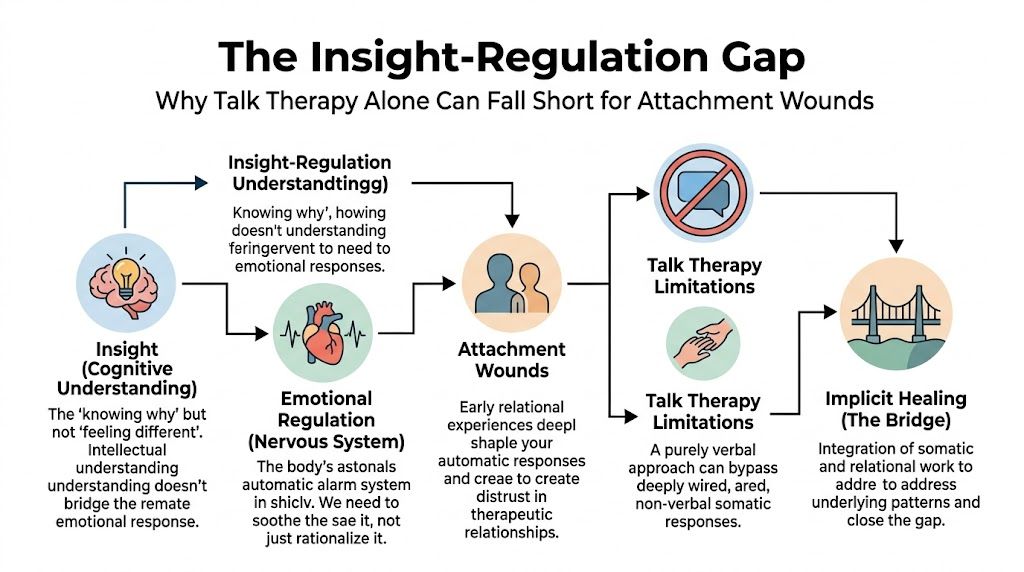
Why insight doesn’t always land
It's like trying to update software on a laptop that’s overheating. The update may be correct. The instructions may be useful. But the machine can’t process them well while it’s under strain.
That’s what happens when someone with attachment trauma enters a threat response. They may know, logically, that their partner’s delayed reply doesn’t mean abandonment. They may understand that setting a boundary isn’t selfish. They may fully agree with everything said in therapy. But if their nervous system is reading the moment as danger, logic won’t lead.
The body gets there first.
For many people with insecure attachment, closeness itself can feel risky. Needing someone can feel risky. Depending on someone can feel risky. Even being deeply seen can feel risky. So a session that looks productive on the surface can still activate hypervigilance, collapse, numbness, or a subtle urge to flee.
Top-down work and bottom-up work
A lot of therapy is top-down. It uses language, reflection, meaning-making, and thought restructuring. These are valuable tools.
Attachment healing often also needs bottom-up support. That includes helping the body notice activation, settle overwhelm, track safety, and tolerate connection without bracing.
What does that look like in practice?
- Top-down work might help you identify that you fear rejection.
- Bottom-up work helps you notice what happens in your chest, breath, jaw, stomach, or impulse to text repeatedly when that fear gets triggered.
- Top-down work says, “This reaction comes from the past.”
- Bottom-up work helps your body stop reacting as if the past is happening right now.
You don’t heal attachment pain only by understanding it. You heal it by having a different experience of safety, connection, and repair.
Why safety changes outcomes
Many therapies often fall short in this particular area. Open Forwards notes that traditional talk therapy often prioritizes cognitive insight, but for clients with attachment trauma, it can activate a dysregulated nervous system without providing tools for somatic repair. The same piece also notes that the therapeutic alliance accounts for 30-50% of outcomes. If your body doesn’t feel safe enough with the therapist, the relationship that should support healing can’t fully form.
That matters because attachment wounds are relational injuries. They don’t usually heal through explanation alone. They heal when your system starts learning, slowly and repeatedly, that connection doesn’t have to cost you yourself.
What doesn’t work and what tends to help
A few common mismatches show up here.
| What often doesn’t work | What tends to help |
|---|---|
| Endless analysis: Session after session of insight with little shift in emotional capacity | Regulation in real time: Slowing down enough to notice activation as it happens |
| Pushing disclosure too early: Going deep before safety exists | Pacing: Building trust before intense processing |
| Staying only in words: Talking about feelings without sensing them | Embodied tracking: Noticing breath, tension, posture, and impulses |
| Treating the pattern as irrational only: Trying to correct it through logic | Respecting protection: Understanding the pattern as a survival strategy first |
If your therapy has felt smart but not leading to real change, the issue may not be motivation. It may be the insight-regulation gap. You know why you react, but your body still doesn’t know how to feel safe enough to do something different.
How Your Attachment Style Shows Up in the Therapy Room
Attachment patterns don’t disappear just because you’re with a trained professional. They usually show up right there in the room.
That’s one reason therapy can feel confusing. A person may sincerely want help while also protecting themselves from the very closeness that healing requires. If you’ve never looked at your patterns through an attachment lens, this attachment style definition guide can help you put language to what you’ve been feeling.

Anxious attachment in therapy
If you lean anxious, therapy can become another place where you monitor the relationship.
You may watch the therapist’s face for signs of disapproval. A neutral expression might feel like distance. A scheduling change might hit as rejection. Silence in the room may feel unbearable, so you fill it quickly. You might also become the “good client” who is insightful, agreeable, and eager to do everything right.
That can look productive. But it can keep the underlying work hidden.
Anxious clients often over-report thoughts and under-report what they fear saying. They may want reassurance more than exploration. They may leave sessions feeling temporarily soothed, then feel destabilized again when life brings the next rupture.
Common therapy-room patterns include:
- People-pleasing the therapist: Saying what sounds mature instead of what feels raw.
- Seeking certainty: Wanting firm answers about the relationship, the future, or whether you’re healing “correctly.”
- Reading into small cues: Tone, pauses, rescheduling, and boundaries can feel loaded.
- Confusing closeness with progress: Feeling attached to the therapist but not necessarily more grounded in your own life.
Avoidant attachment in therapy
Avoidant attachment often looks very different. These clients can be articulate, thoughtful, and easy to mistake for regulated.
They may tell the story cleanly, with insight and precision, while staying far away from felt experience. Their therapy can become a seminar on their life rather than a contact point with it. They know what happened. They just don’t stay with what it did to them.
When therapy gets more emotionally intimate, they may downplay the issue, become skeptical, go blank, or suddenly decide they don’t need therapy after all.
Watch for signs like these:
- Staying intellectual: Talking about emotions instead of from within them.
- Minimizing pain: “It wasn’t that bad” or “other people had it worse.”
- Disconnecting under closeness: Feeling irritated, tired, numb, or mentally checked out.
- Quitting at the edge of change: Wanting to leave therapy when the work starts feeling vulnerable.
Avoidant patterns don’t always say “I’m scared.” They often say, “This isn’t necessary.”
Disorganized attachment in therapy
Disorganized attachment is often the most distressing because it holds opposite drives at once. You want closeness and fear it. You long to be understood and don’t trust the person trying to understand you.
In therapy, this can create a push-pull dynamic. One week you feel profoundly connected and relieved. The next week you feel suspicious, exposed, angry, or convinced the therapist doesn’t get you at all. You may share something vulnerable and then feel regret, shame, or panic afterward.
This isn’t inconsistency for its own sake. It’s a protection system built around conflict. The relationship feels like the solution and the threat.
Disorganized patterns often include:
- Rapid shifts: Feeling attached, then wanting to pull away.
- Difficulty trusting the process: Even when therapy helps, another part expects harm.
- Strong rupture sensitivity: Small misunderstandings can feel enormous.
- Inner confusion: Not knowing whether to reach out, hide, protest, or disappear.
Why naming the pattern helps
Once you understand how your attachment style shows up in therapy, your reactions stop looking random. They become readable. That changes everything.
Instead of saying, “I’m impossible to help,” you can start saying, “My protection system is active.” That creates room for compassion, better pacing, and a more targeted kind of support.
Finding a Therapist Who Truly Sees You
For attachment healing, the therapist isn’t just delivering a method. The relationship itself is part of the treatment.
That doesn’t mean you need perfect chemistry or constant warmth. It means your system needs enough safety, steadiness, and responsiveness to let down some of its guard. Without that, the work stays performative, detached, or overwhelming.

Competent is not the same as attuned
A therapist can be educated, ethical, and skilled on paper, yet still not be the right fit for attachment work.
A clinically correct therapist may reflect accurately, ask appropriate questions, and maintain boundaries well. An attuned therapist does that and also tracks your pace, notices subtle shifts in your state, responds to ruptures, and helps you stay within a range where you can feel without flooding or shutting down.
That difference matters. Alma’s survey found that 39% of people ended therapy primarily because of a lack of connection with their therapist. If you’ve left therapy feeling unseen, that experience deserves to be taken seriously.
Signs of a good fit for attachment work
You’re not looking for someone who says all the right buzzwords. You’re looking for someone whose presence helps your system settle enough to be real.
Good signs include:
- You feel felt: The therapist seems to grasp not just the content of your story, but the emotional logic underneath it.
- You can be imperfect: You don’t feel pressure to perform insight, be likable, or package your pain neatly.
- They don’t rush depth: They build safety before asking you to revisit highly charged material.
- They can repair strain: If you feel misunderstood, they can stay open and work through it with you.
- Your body gives useful feedback: You may still feel activated, but not chronically braced, shamed, or abandoned in the room.
Red flags people often ignore
Clients with attachment wounds are especially prone to overriding their instincts. They may stay with a therapist because they “should,” because the therapist is nice, or because leaving feels like failing.
Pay attention if you consistently notice:
- Feeling judged or subtly corrected
- Feeling more exposed than supported
- Repeatedly leaving sessions flooded with no help settling
- A therapist who insists on vulnerability before trust exists
- A sense that your reactions are being analyzed more than understood
If your body keeps saying “not safe,” don’t force yourself to call it resistance.
What attunement feels like
Attunement doesn’t always feel dramatic. Often it feels simple. You exhale more fully. You don’t have to explain every layer for them to get the core of it. You feel less alone with yourself.
That’s not a luxury in attachment work. It’s the ground the work stands on.
Your Action Plan for Finding Therapy That Works
When therapy hasn’t helped, starting over can feel exhausting. It also gives you valuable information. You now know that insight alone may not be enough, and that your attachment pattern can shape what happens in the room.
That means your next search can be more precise.
Mainstream discussions of therapy failure often miss how attachment patterns interfere with progress and why insight-based work may fall short without nervous system support. That gap matters when you’re trying to choose your next step.
Start with better search terms
A generic therapy search often leads to generic treatment. If you suspect attachment wounds, use language that points toward relational and body-based work.
Search terms that can help:
- Attachment-focused therapist
- Trauma-informed therapist
- Somatic therapy
- Somatic Experiencing
- EMDR
- Polyvagal-informed therapist
- Parts work
- Internal Family Systems
- Relational therapy
- Nervous system regulation therapist
If you’ve spent years in cognitive work with little change, this article on the limitations of cognitive behavioral therapy may help you clarify what felt missing.
Read therapist websites like a filter, not a brochure
A therapist’s website can tell you a lot before you ever book a call.
Look for language that suggests they understand more than symptom management. Strong signs include references to trauma, attachment, emotional regulation, relational patterns, pacing, safety, or embodied healing. If every sentence sounds polished but vague, keep looking.
It also helps to notice what’s absent. If the entire approach is framed around changing thoughts, improving productivity, or solving present-day stress without any mention of the body or relationship history, that may not be enough for attachment-focused work.
What different modalities may feel like
Many people know the names of therapies but not what they look like in practice.
Here’s a simple comparison:
| Modality | What it often focuses on | What it may feel like in session |
|---|---|---|
| Attachment-focused therapy | Relational patterns, emotional needs, safety, trust, rupture and repair | Exploring how your past shows up between you and the therapist, partner, or others |
| Somatic therapy | Body cues, activation, settling, felt sense, unfinished survival responses | Slowing down to notice breath, tension, impulses, and sensations while staying grounded |
| EMDR | Reprocessing distressing experiences in a structured way | Working with specific memories, present triggers, and internal shifts |
| Parts work | Different inner states or protective strategies | Naming the part that chases, the part that shuts down, the part that feels ashamed, then relating to each differently |
Use the connection call to interview them
You are not asking for permission to be helped. You are assessing fit.
Use the consultation call to hear how a therapist thinks, not just what they list in their profile.
| Question Category | What to Ask | What to Listen For |
|---|---|---|
| Attachment knowledge | “How do you work with anxious, avoidant, or disorganized attachment?” | Specific, clear language about patterns in relationships and therapy itself |
| Nervous system support | “What do you do when a client gets overwhelmed, shut down, or highly activated in session?” | A plan for pacing, grounding, and regulation rather than pushing through |
| Therapeutic relationship | “How do you handle it if I feel misunderstood or disconnected from you?” | Openness to rupture and repair, not defensiveness |
| Modality fit | “How would your approach help someone who understands their patterns but still reacts automatically?” | A response that goes beyond insight and includes body-based or experiential work |
| Pacing and safety | “How do you decide when to go deeper into hard material?” | Respect for readiness, consent, and building enough stability first |
| Measuring progress | “How will we know therapy is helping?” | Concrete markers like better regulation, clearer boundaries, less reactivity, stronger self-trust |
Listen for these phrases and attitudes
A good answer usually sounds grounded and flexible. A weak answer often sounds generic.
Encouraging signs:
- They mention regulation, pacing, or safety
- They expect attachment patterns to show up in therapy
- They speak respectfully about protectors like numbness, overthinking, or people-pleasing
- They seem comfortable with complexity rather than trying to force a quick fix
Be cautious if they dismiss body-based work, seem irritated by questions, or treat your history as interesting content rather than lived conditioning.
Keep your first goal modest
Your first goal doesn’t need to be “heal everything.” Start smaller.
Aim for this: find someone with whom you feel curious, not collapsed. Someone whose approach makes sense to your whole system, not just your intellect. Someone who helps you become more real, not more polished.
That’s often where healing finally starts moving.
Healing Beyond the Therapy Room Your Nervous System Toolkit
Therapy matters. What you practice between sessions matters too.
If your system has learned to brace for disconnection, then small moments of regulation outside therapy help build a new baseline. These are not tricks to suppress emotion. They are ways to help your body come out of automatic threat long enough to choose a response.
If you want a fuller foundation, this guide to nervous system regulation can help you understand what your body is doing and why.

Orienting
This is one of the simplest tools, and it’s especially helpful when you feel suddenly tense, frozen, or hyper-alert.
Try this slowly:
- Let your eyes look around the room.
- Notice a few neutral or pleasant objects.
- Name them to yourself. Lamp. Window. Mug. Blue blanket.
- Let your neck move gently as your eyes scan.
- Notice whether your breath changes on its own.
Why it helps: orienting tells the brainstem that you are in the present environment, not trapped in an old threat. It interrupts tunnel vision and brings in new information.
Ground through contact
When people are overwhelmed, they often float upward into thoughts. Grounding brings attention back to support.
You can do this almost anywhere:
- Feet on the floor: Press down gently and notice the contact.
- Back in the chair: Feel the surface holding your weight.
- Hands together: Rub your palms or hold one hand with the other.
- Name the support: “The chair is here. The floor is here. I am being held up.”
Why it helps: your body responds to contact cues. Support is not only an idea. It is something your nervous system can register directly.
Try not to ask, “Is this working yet?” Ask, “Can I stay with this for one more breath?”
The physiological sigh
This is a useful reset when you feel keyed up, panicky, or like your body is revving too fast.
How to do it:
- Inhale through your nose.
- Take a second small inhale on top of the first.
- Exhale slowly through the mouth.
- Repeat a few times, gently.
Why it helps: the extended exhale supports down-regulation. It gives your system a direct cue that it can come down from high activation.
A simple journaling shift
Journaling helps many people. But if you only use it to analyze, you may stay in the same loop. Try changing the prompt.
Instead of “Why am I like this?” try:
- What happened right before I got activated?
- What did my body do first?
- What did I need in that moment?
- What helped even a little?
That kind of journaling builds pattern recognition without turning into self-criticism.
If you’d like guided support, embed one of your own regulation videos from the @SecurelyLoved channel here, such as a short practice on grounding or calming the nervous system. Use a video that demonstrates one technique slowly and clearly so readers can follow in real time.
Keep the bar low and repeatable
The most effective regulation tools are usually the ones you’ll use. Not the ones that sound impressive.
Choose one practice and repeat it at predictable moments. After a hard conversation. Before opening a message that makes you nervous. When you notice yourself rehearsing, chasing, or shutting down. Repetition teaches safety better than intensity does.
You Can Feel Safe and Seen on Your Healing Journey
If therapy hasn’t worked the way you hoped, that pain is real. It can make you doubt yourself, your history, and the whole idea of healing. But your past therapy experiences are not proof that you can’t get better. They are data.
They may be telling you that you need a method that reaches beyond insight. They may be telling you that your attachment pattern has been running the room more than anyone realized. They may be telling you that safety, pacing, and attunement are not extras for you. They are the treatment.
That changes the question from “Why am I not responding?” to “What kind of support helps me feel safe enough to respond?”
There’s also value in building a wider support plan while you do this work. Some people explore sleep support, nutrition, movement, or calming routines alongside therapy. If you’re curious about complementary options, this overview of stress relief supplements offers a practical starting point for understanding one piece of that larger picture.
You do not need to force yourself through more of what already feels misaligned. You can choose a different kind of help. You can learn your nervous system. You can find a therapist who doesn’t just hear your words, but understands your protective patterns and knows how to work with them.
Healing often begins when you stop treating your reactions like defects and start reading them as intelligent adaptations that are finally ready for care.
If you’re ready for a gentler, more attachment-focused path, Securely Loved offers therapy and resources designed for adults who feel stuck in repeating patterns, emotional overwhelm, or the aftermath of inconsistent emotional attunement. You can explore the site’s learning tools or book a free connection call to see whether this kind of support feels like a fit.
