
Cognitive behavioral therapy for anxious attachment: Cogniti
Your phone lights up. It’s not the message you were hoping for.
Maybe there’s no message at all.
You tell yourself to be normal about it. Give it time. Stay busy. But within minutes, your mind is moving faster than your body can keep up. They’re pulling away. I said too much. I care more than they do. I’m about to be abandoned again.
Then the behaviors follow. You reread the last exchange. You check their social media. You draft a text, delete it, send a different one, regret that one too. Part of you knows this spiral is hurting you. Another part feels certain that if you don’t act right now, you’ll lose the connection.
If this is familiar, you’re not needy, broken, or too much. You’re likely caught in an anxious attachment pattern, and those reactions make sense when your system learned early that closeness could feel uncertain.
Cognitive behavioral therapy for anxious attachment can help because it gives you a structure for interrupting the spiral. Not by shaming your feelings. Not by telling you to “just be less sensitive.” It helps you slow down, identify what your mind is predicting, and respond in a more grounded way.
That matters because anxious attachment rarely changes through insight alone. Many individuals already know they’re overthinking. The hard part is catching the pattern in real time and doing something different when your fear feels urgent and believable.
CBT gives you that practical middle step between trigger and reaction.
The Anxious Attachment Spiral and A Path Forward
A delayed text is rarely just a delayed text when you have anxious attachment.
It can feel like a referendum on your worth, your safety, and the future of the relationship. One small gap in communication becomes a full internal crisis. Your mind fills in missing information with the most painful explanation available.
When the spiral takes over
A lot of people I work with describe the same sequence.
First, there’s a moment of uncertainty. A shorter reply. A canceled plan. A partner who seems distracted. Then comes the emotional surge. Tight chest. Restlessness. Racing thoughts. The urgent need to fix, clarify, or secure the bond.
From there, the spiral often sounds like this:
- Catastrophic thinking: “They’re losing interest.”
- Mind reading: “They must be annoyed with me.”
- Self-blame: “I ruined this.”
- Protective behavior: repeated texting, overexplaining, withdrawing, or seeking reassurance
None of this happens because you lack intelligence or self-awareness. It happens because your attachment system is trying to prevent loss.
Anxiety in relationships often looks irrational from the outside. Inside your body, it feels like an emergency.
Why CBT helps
CBT is useful here because it’s concrete.
It helps you identify the exact thought that kicked off the spiral, the feeling that followed, and the behavior you used to cope. Once you can see that sequence, you can start changing it.
That doesn’t mean you stop caring. It means you stop handing your nervous system over to every ambiguous moment.
For attachment-related anxiety, CBT works especially well as a foundational treatment because it targets the patterns that keep fear going. In a significant randomized trial of anxious adolescents, 67% of those in the CBT-only group no longer met criteria for their primary anxiety diagnosis after treatment, and that rose to 100% at follow-up according to the PubMed study on CBT for adolescent anxiety.
A more grounded path
The first shift is often simple, but powerful. You stop asking, “What’s wrong with me?” and start asking, “What did my mind just tell me, and what did I do next?”
That question creates room.
Room to pause. Room to reality-check. Room to respond with skill instead of panic. And over time, room to build something anxious attachment often lacks internally, which is a felt sense of steadiness.
How CBT Maps onto Your Anxious Attachment Patterns
Anxious attachment works like an overactive relationship alarm system.
It developed for a reason. At some point, staying alert to shifts in connection may have helped you stay close, avoid conflict, or protect yourself from emotional pain. The problem is that this alarm system often keeps firing long after the original conditions are gone.

Your alarm system isn’t the enemy
If your partner says, “I’m busy today,” your attachment alarm may translate that into, “I’m being left.”
That jump can feel instant. You don’t sit down and choose it. Your body reacts first, and your mind races to explain why.
CBT helps by making those fast internal moves visible.
The thoughts, feelings, and behaviors loop
At the center of cognitive behavioral therapy for anxious attachment is a simple idea. Thoughts, feelings, and behaviors affect each other.
Here’s what that can look like in real life:
| Situation | Thought | Feeling | Behavior |
|---|---|---|---|
| Your partner hasn’t replied for hours | “They’re losing interest” | panic, sadness, dread | multiple texts, checking their activity, inability to focus |
| Someone you’re dating seems less expressive than usual | “I did something wrong” | shame, anxiety | overexplaining, people-pleasing, replaying the conversation |
| Your partner asks for space after conflict | “Space means abandonment” | fear, urgency | pushing for immediate resolution, calling repeatedly, crying, shutting down later |
The key point is this. The behavior usually makes temporary anxiety feel smaller, but it often makes the overall pattern stronger.
If you text five times and get reassurance back, your brain learns, panic worked. If you overanalyze all night and your partner is kind in the morning, your brain learns, hypervigilance protected me. CBT interrupts that learning loop.
Where change becomes possible
You don’t have to fix everything at once. You just need an effective point of influence.
In CBT, there are usually three strong places to intervene:
- At the thought level: question the story your mind generated
- At the emotional level: name what you feel instead of becoming it
- At the behavior level: choose one different action, even if your anxiety is still loud
This is why CBT often gives a sense of agency to people with anxious attachment. It doesn’t ask you to wait passively until you magically feel secure. It gives you a method.
Practical rule: If your reaction feels urgent, that’s often the moment to slow the process down, not speed it up.
A gentler way to interpret your reactions
Many people with anxious attachment shame themselves for being reactive. That shame usually adds another layer of distress. A better frame is this: your system is overpredicting danger in relationships.
That’s very different from being defective.
Once you understand the pattern, you can start to separate a trigger from the meaning your mind assigned to the trigger. That separation is where secure behavior begins.
Practical CBT Exercises to Soothe Relationship Anxiety
When CBT works, it doesn’t feel abstract. It feels usable on a Tuesday night when your chest is tight and you’re fighting the urge to send one more text.
Clients often notice measurable progress with CBT in 12-20 sessions, and some report an early shift in awareness and trigger management within the first 4-8 weeks, as described in this piece on CBT for anxious attachment style. The point isn’t instant perfection. The point is that change becomes observable.

Exercise one, catch and rework the thought
This is classic cognitive restructuring, but it needs to be practical.
Start with a recent trigger. Don’t choose your most overwhelming one first. Pick something manageable.
Write down:
What happened
“They read my message and didn’t reply for three hours.”What I told myself
“They’re annoyed. I’m too much. This is going badly.”What I felt
“Panicked, rejected, embarrassed.”What I did
“Checked my phone constantly. Sent a follow-up text.”A more balanced thought
“A delayed reply can mean many things. I don’t have enough information yet.”
Balanced doesn’t mean fake-positive. It means credible.
If you’ve been spiraling around infidelity fears or scanning for hidden signs, a grounded resource on anxiety about partner cheating can help you sort the difference between fear-driven pattern detection and legitimate concern.
Exercise two, run a behavioral experiment
Anxious attachment makes predictions all day long.
If I don’t check in, they’ll forget about me.
If I don’t fix this now, the relationship will fall apart.
If I stop asking for reassurance, I’ll feel worse forever.
A behavioral experiment tests one prediction instead of obeying it.
Try this small experiment
You usually send a second text after 10 minutes of no response. This time, wait longer.
Before you do it, write:
- Prediction: “If I don’t send another text, they won’t care.”
- Plan: “I will wait before following up and observe what happens.”
- What happened: Fill this in later, not in your head
One commonly used example in attachment-focused CBT is delaying reassurance-seeking to see whether the feared outcome occurs. The goal isn’t to suppress needs. It’s to gather real evidence.
Most anxious predictions feel convincing because they’re familiar, not because they’re accurate.
Exercise three, use exposure with a communication script
Uncertainty is part of relationships. Anxious attachment treats uncertainty like danger.
Exposure means you practice staying present with a tolerable amount of uncertainty instead of immediately escaping it through control, protest, or self-abandonment. With relationships, exposure often works best when paired with clear communication.
A simple script
Try this when you feel activated but want to stay connected:
“I’m feeling anxious today, and I notice I’m wanting extra reassurance. I’m going to slow myself down first, but I also wanted to let you know what’s happening for me.”
That kind of statement is different from protest behavior. It’s honest, regulated, and specific.
If your body is too activated to speak clearly, use grounding first. These grounding techniques for trauma can help you settle enough to choose your next step instead of reacting from panic.
A short practice sequence
Use this when you feel the spiral start:
- Name the trigger: “They got quiet after dinner.”
- Name the story: “My mind says I’m being rejected.”
- Pause the impulse: put the phone down, stand up, drink water
- Ground your body: longer exhale, feet on floor, orient to the room
- Choose one intentional action: wait, journal, or send one clear message instead of several
If you’d like a guided teaching piece from Bev Mitelman, embed a video from the @SecurelyLoved YouTube channel here that walks through one grounding or thought-challenging exercise for relationship anxiety.
CBT for Anxious Attachment in Everyday Life Two Vignettes
Theory matters. What usually changes people is seeing how this looks in ordinary life.
Sarah in early dating
Sarah is in her 30s, bright, capable, and outwardly calm. Internally, dating feels like being skinned alive.
She meets someone she likes. Their first few dates go well. Then one evening he doesn’t respond until the next morning. By midnight, she’s already moved through five different explanations, and all of them end with rejection.
Her first thought is, I opened up too much. Her second is, I should pull back before he does. Historically, that’s what she’s done. She’d either send a tense, overcareful message or disappear for a few days while obsessing.
This time she uses a CBT worksheet instead.
What changed for Sarah
She identifies the automatic thought: He’s losing interest.
Then she asks three questions:
- What facts support this?
- What facts don’t support it?
- What’s another explanation that fits the situation?
She realizes she has one fact only. He hasn’t replied yet. She does not have evidence of rejection.
Then she does a behavioral experiment. Instead of sending a follow-up text to force clarity, she waits and notices what happens in her body. She journals the urges. She goes for a walk. The next morning, he replies warmly and apologizes for a late work issue.
That didn’t magically cure her attachment anxiety. What it did was weaken the certainty of her old story. She learned that discomfort and danger aren’t always the same thing.
Michael in a long-term relationship
Michael has been with his partner for years. Their recurring conflict is about space.
Whenever his partner says, “I need some time to think,” Michael hears, I’m leaving you emotionally. He follows her from room to room, pushes for immediate resolution, and gets louder as he gets more afraid. Afterward, he feels ashamed and confused about why he couldn’t stop.
He doesn’t need more insight into childhood. He already has plenty. He needs a way to interrupt the escalation when it starts.
What changed for Michael
He begins by tracking the sequence after conflict.
His trigger is distance. His thought is, If we don’t fix this now, the relationship is unsafe. His feeling is panic. His behavior is pursuit.
Once he can see the sequence, he builds a replacement plan.
When his partner asks for space, he says: “I notice I’m getting activated and wanting to keep talking. I’m going to take a pause too. Can we come back to this later today?”
That sentence took practice. The first few times, he said it while still visibly tense. But he said it.
Then he used a self-soothing routine during the pause. Slow breathing. Writing down his catastrophic thoughts. Reminding himself that space after conflict is not the same as abandonment.
Secure behavior often looks ordinary. One clear sentence. One pause. One less reactive choice.
What changed most for Michael wasn’t his need for connection. It was his ability to stay in connection without turning panic into pressure.
These are the kinds of shifts CBT can support. Not perfect calm. Better recovery. More reality-testing. Less automatic escalation.
Beyond Thoughts Why Integrating the Nervous System is Key
Some people try cognitive behavioral therapy for anxious attachment and come away frustrated.
They understand the thought work. They can name the distortion. They can even generate a balanced belief. But their body still feels like it’s falling off a cliff.
That doesn’t mean they failed CBT. It means cognition isn’t the whole story.
Why thought work sometimes doesn’t stick
Attachment anxiety is often very physical.
Your jaw tightens. Your stomach drops. Your heart races. You feel an urge to cling, explain, collapse, or chase. If your nervous system is in a survival state, a rational thought may be true and still not feel believable.
That’s where an integrated approach matters.
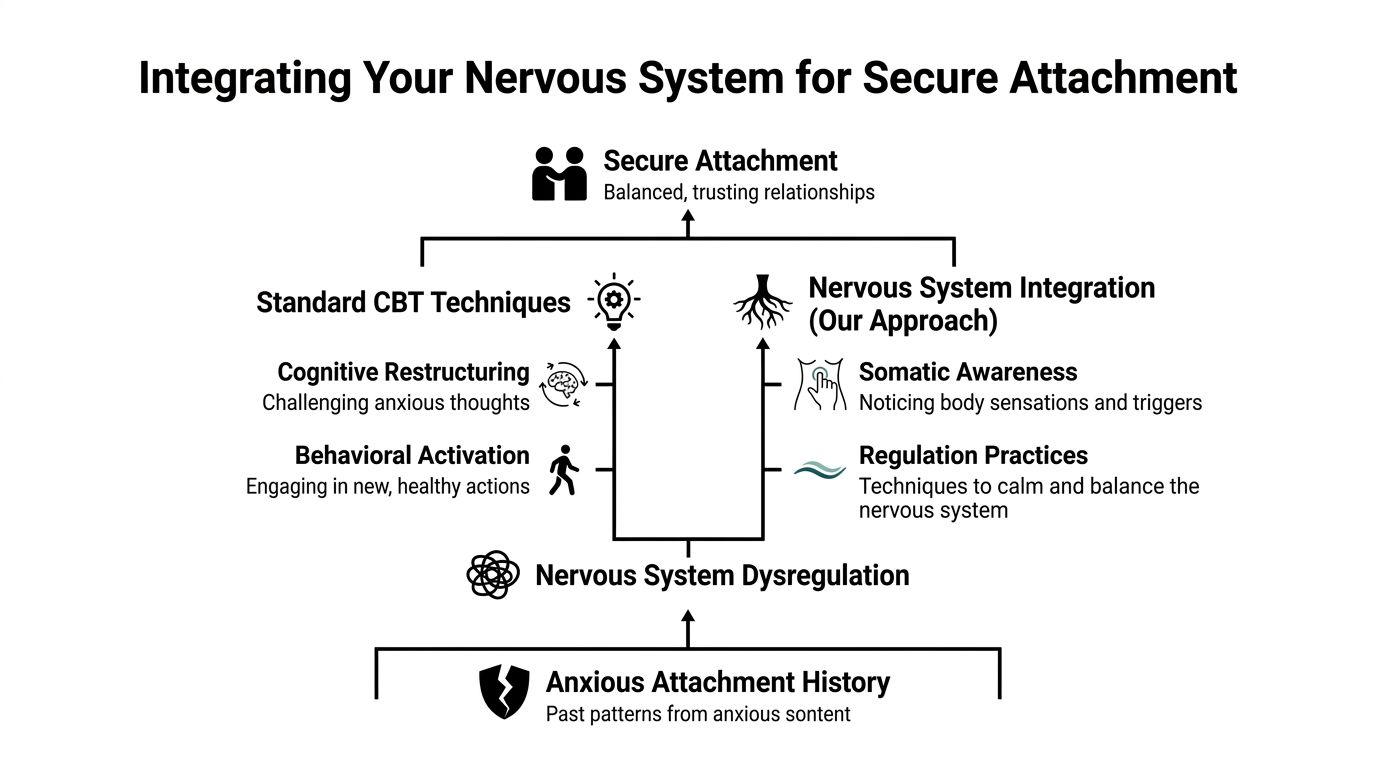
The missing layer for many people
Research and clinical discussion increasingly point to a gap in standard CBT-only approaches for attachment-based distress. This review on integrated, trauma-informed approaches for attachment-related anxiety notes that for attachment-based issues, integrated models can yield better outcomes and that anxiety must be understood in relational and embodied terms, not only as distorted thinking.
That fits what many clients already know from experience. You can’t always out-think a body that feels endangered.
What nervous system aware CBT looks like
It still includes CBT tools. You still challenge abandonment stories. You still test anxious predictions. You still work on behaviors that keep the cycle alive.
But you also add regulation.
That might include:
- Somatic awareness: noticing throat tension, shallow breathing, collapse, or agitation before the spiral fully takes over
- State tracking: learning the difference between a grounded need and a threat-driven demand
- Body-based settling: orienting, longer exhales, pressure, movement, or other practices that help your system come back online
If you’re curious about concrete body-based options, this guide to vagus nerve stimulation techniques can offer practical starting ideas. For a deeper attachment-focused lens, this resource on nervous system regulation therapy connects regulation work directly to relationship healing.
When your body feels safer, your mind becomes more teachable.
What this changes in practice
Without nervous system support, CBT can turn into a mental wrestling match.
You keep trying to reason with panic while panic keeps winning. With regulation in the mix, you create enough internal stability for the cognitive work to land. Then your balanced thought is no longer just intellectually correct. It becomes emotionally possible.
This is especially important for people who’ve done years of traditional talk therapy and still feel hijacked in close relationships. Often, they don’t need more insight. They need a method that respects how attachment fear lives in the body.
Is CBT the Right Therapy for Your Attachment Style
You read a shorter-than-usual text from your partner, feel your chest tighten, and spend the next hour trying to figure out what changed. If that pattern is familiar, CBT may give you a clear place to start.
CBT tends to work well for anxious attachment when your distress follows a pattern you can name. A trigger happens. Your mind fills in the blanks. You act from fear, then regret it later. If that sequence sounds familiar, structured cognitive work can help you interrupt it sooner and respond with more choice.
Signs CBT may fit well
CBT is often a good match if these patterns describe you:
- You get pulled into predictable thought loops: replaying texts, assuming the worst, mind reading, or catastrophizing
- You like structure: worksheets, experiments, scripts, and between-session practice feel useful
- You can reflect once the moment passes: even if you get activated quickly, you can usually trace what set you off
- You want tools, not just insight: you want help changing the pattern, not only understanding where it came from
I often recommend CBT first when someone needs traction fast. It gives language to the spiral and a method for working with it. For many people, that creates real relief.
It also has limits.
When CBT is helpful, but not sufficient on its own
If your attachment anxiety comes with dissociation, trauma flashbacks, shutdown, or intense body panic, CBT may not be enough by itself. You may understand the thought distortion perfectly and still feel completely overtaken in the moment.
That does not mean you are failing therapy. It usually means your nervous system needs treatment too.
For deeper and more lasting change, CBT often works best as one part of a broader plan that includes trauma-informed care and body-based work. If you want a clearer picture of where cognitive tools can fall short by themselves, this article on the limitations of cognitive behavioral therapy explains the gap well.
Choosing Your Therapy Path for Anxious Attachment
| Therapy Type | Primary Focus | Best For… | Typical Format |
|---|---|---|---|
| CBT | thoughts, behaviors, triggers, coping skills | people with repetitive anxious thought patterns who want concrete tools and structure | present-focused sessions with exercises, tracking, and between-session practice |
| EMDR | trauma processing and reprocessing distressing memories | people whose attachment anxiety links strongly to unresolved trauma memories | structured trauma-focused sessions led by a trained clinician |
| Somatic Experiencing | body sensations, survival responses, regulation | people who feel attachment anxiety mainly as physical overwhelm, shutdown, or activation | slower paced sessions centered on body awareness and nervous system regulation |
The trade-off is straightforward. CBT gives clarity and repetition. Trauma and somatic therapies often move more slowly, but they can reach the layers that insight alone does not touch. Some people need one primary approach. Many do best with an integrated plan.
A note for midlife women
Perimenopause and menopause can intensify attachment anxiety in ways that feel confusing and discouraging. A woman may have done solid therapy, built real self-awareness, and still find herself more reactive, more vigilant, or less resilient during this stage of life.
CBT can still help here because it offers structure when your internal experience feels less predictable. But I would not rely on cognitive tools alone if your body is already under strain from hormonal shifts, sleep disruption, or chronic stress. In that season, the strongest treatment plan usually includes CBT plus nervous system support, and often a wider look at your physical health.
The right therapy fits your patterns, your history, and the way your body responds under stress. If standard talk therapy has helped you understand yourself but has not changed what happens in close relationships, that is useful information. It often means you need more than insight. You need an approach that works with both the story in your mind and the alarm in your body.
Your First Step Toward a More Secure You
Anxious attachment can make love feel exhausting. You overread, overfunction, overexplain, and still end up feeling alone inside the relationship.
That pattern can change.
Cognitive behavioral therapy for anxious attachment gives you a way to catch the spiral, question the old story, and choose behaviors that create more stability. For many people, that’s the first major turning point. For deeper healing, the work often becomes even more effective when you include nervous system regulation and somatic support alongside the cognitive tools.
You do not need to wait until you’re in another crisis to begin. You also don’t need to have the perfect explanation for why you react the way you do.
Two gentle next steps can help:
- Take an attachment style quiz if you want language for what’s been happening in your relationships
- Book a free 15-minute connection call if you want a private space to talk through your goals and what kind of support might fit
Healing usually doesn’t begin with one giant breakthrough. It starts with one honest moment of seeing the pattern clearly, and one supported step in a new direction.
If you’re ready for support, Securely Loved offers attachment-focused, trauma-informed care for adults who feel stuck in anxious, avoidant, or disorganized relationship patterns. You can explore resources, take the attachment style quiz, or book a free 15-minute online connection call to find a compassionate next step.
