
Cognitive behavioral therapy for anxious attachment style: C
You check your phone again. Nothing.
A few minutes ago, your partner sounded slightly off in a text, or said they needed space, or ended a call faster than usual. Since then, your mind has been doing what anxious attachment does so well. Scanning. Interpreting. Predicting. Preparing for loss before anything has happened.
By now, you may know this pattern intellectually. You may already understand that your fear of abandonment gets activated fast. But insight alone often doesn't stop the wave. Your chest still tightens. Your stomach drops. You still want to text again, ask if everything is okay, replay the conversation, or shut down before you can be left.
That’s where cognitive behavioral therapy for anxious attachment style can help. CBT gives you a clear way to identify the thoughts, emotions, and behaviors that keep relationship anxiety going. It helps you slow the spiral and respond differently.
But I want to say something many people need to hear. If you've tried to “think your way out” of attachment panic and it hasn’t worked, you’re not doing it wrong. Many resources leave out the body. Existing content on CBT for anxious attachment often underplays nervous system regulation, even though some people feel emotionally flooded despite having solid cognitive insight. One article summarizing this gap notes that a 2025 Frontiers in Psychology study found schema-integrated CBT may accelerate shifts toward secure attachment by targeting amygdala reactivity, while practical combinations of CBT and polyvagal-informed exercises are still rarely spelled out in detail in this discussion of cognitive behavioral therapy for anxious attachment style.
That’s the bridge this guide is meant to offer. Not just better thoughts. Embodied safety.
The Unseen Work of an Anxious Heart
You might look calm on the outside and still feel like your whole inner world is on fire.
I see this often. Someone is successful, caring, insightful, and capable in most parts of life. But in close relationships, one delayed reply can unravel their sense of safety. They don’t become dramatic. They become desperate for certainty.

What anxious attachment feels like from the inside
Anxious attachment rarely feels irrational when you're in it. It feels urgent. It feels protective. It feels like your system is trying to save an important bond.
That’s why simple advice like “just calm down” or “don’t overthink it” usually lands badly. The problem isn't a lack of intelligence. The problem is that your attachment system has learned to treat disconnection like danger.
Common moments that set it off include:
- A change in tone: A shorter text, a delayed reply, less enthusiasm than usual.
- A bid for space: Your partner says they’re tired, overwhelmed, or need time alone.
- An unclear interaction: Nothing explicit went wrong, but you feel a shift and start searching for what it means.
- A memory trigger: This relationship is fine, but your body reacts as if an old abandonment is happening again.
If you want a deeper foundation for recognizing these patterns, this overview of understanding anxious attachment styles can help put language to what you’re living.
Why CBT matters here
CBT works well for attachment anxiety because it is practical. It doesn’t ask you to stay in vague reflection forever. It asks what happened, what you told yourself, what you felt, what you did next, and whether that pattern helped or harmed you.
You are not “too much” because your nervous system learned to anticipate inconsistency.
The unseen work of an anxious heart is exhausting because so much of it happens in milliseconds. A trigger appears. A belief snaps into place. Your body mobilizes. Then your behavior tries to close the gap between fear and relief.
CBT helps make that sequence visible. Once you can see it, you can begin to interrupt it.
How CBT Interrupts the Anxious Attachment Cycle
CBT becomes powerful when you stop seeing your anxiety as random and start seeing it as a sequence.
For anxious attachment, that sequence is often painfully predictable. A relationship cue gets interpreted as threat. A core fear gets activated. Your body reacts. Then your behavior tries to restore safety quickly, even if the strategy creates more instability later.

Research supports this structured approach. One summary reports that CBT significantly reduced attachment anxiety in 10 weeks, with many people noticing progress within 12 to 20 sessions in this review of therapy for anxious attachment.
The cycle in plain language
Here’s a common anxious attachment loop:
Trigger
Your partner says, “I’m wiped tonight. I’ll text tomorrow.”Meaning
Your mind fills in the blanks.
“They’re pulling away.”
“I did something wrong.”
“I’m too needy.”Emotion and body reaction
Panic, dread, sadness, agitation. Tight chest. Nausea. Restlessness.Protective behavior
Sending another text. Checking social media. Replaying the conversation. Asking for reassurance. Going cold to regain control.Short-term relief, long-term cost
Maybe you get a reply and feel better briefly. But your brain learns that anxiety must be solved immediately, not tolerated and examined.
What CBT changes
CBT doesn’t start by arguing with your feelings. It starts by identifying the thought-behavior loop that’s intensifying them.
That distinction matters.
If the thought is “I’m about to be abandoned,” your body will respond as if danger is present. If the behavior that follows is repeated reassurance-seeking, your brain gets the message that the threat was real enough to require urgent action.
CBT works by breaking that automatic chain.
A relatable example
Let’s say Maya notices her partner has read her message and not responded.
Her old pattern looks like this:
| Step | What happens |
|---|---|
| Trigger | Seen message, no reply |
| Thought | “He’s upset with me” |
| Feeling | Anxiety, shame, fear |
| Behavior | Sends two follow-up texts, then withdraws hurt |
| Result | Temporary relief if he replies, deeper insecurity if he doesn’t |
A CBT lens helps Maya ask better questions:
- What facts do I have?
- What story did my attachment system add?
- What am I feeling in my body?
- What urge am I trying to discharge?
- What would a steadier response look like?
CBT is not self-blame
Some people resist CBT because they think it means, “Your thoughts are wrong, so just be more logical.”
That’s not good CBT. Good CBT is compassionate and precise.
It recognizes that anxious attachment beliefs usually formed for a reason. If closeness once felt inconsistent, your mind learned to stay alert. The work isn't to shame that adaptation. The work is to update it.
Practical rule: Name the trigger before you name the catastrophe. “My partner is quiet tonight” is more accurate than “I’m being abandoned.”
Core beliefs beneath the spiral
Most anxious attachment reactions are powered by a few familiar beliefs:
- “I’m too much.”
- “If someone needs space, they’ll leave.”
- “I have to earn closeness.”
- “If I’m not wanted right now, I’m not safe.”
CBT helps you recognize that these are not facts. They are learned interpretations.
When you work with them directly, you stop treating every relationship moment like final proof of your deepest fear. That shift is where healing begins.
Your Practical CBT Toolkit for Relationship Anxiety
Insight is useful. Tools change patterns.
The most effective CBT tools for anxious attachment are the ones you can use in the exact moment your mind starts writing a painful story. Not three hours later. Not only in therapy. Right there, in the text thread, after the tense conversation, during the wait.
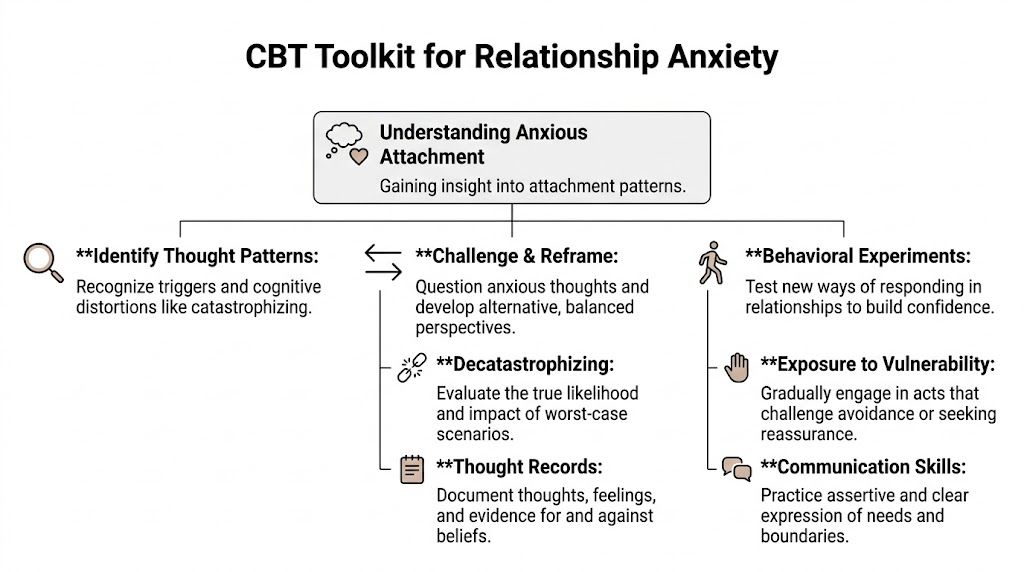
Start with an attachment-focused thought record
A standard thought record is helpful. An attachment-focused one is better because it captures the relationship trigger, the abandonment story, and the urge that follows.
Use this simple table when you feel activated:
| Situation | Anxious Thought | Feeling | Secure Reframe |
|---|---|---|---|
| Partner said they need a quiet night | “They’re losing interest” | Panic, sadness | “A need for space isn’t the same as rejection” |
| Text reply was short | “They’re mad at me” | Fear, shame | “Short messages can reflect stress, fatigue, or distraction” |
| They didn’t initiate today | “I’m not important to them” | Anxiety, loneliness | “One day of lower contact doesn’t define the relationship” |
What to write down
Keep it concrete.
- Situation: Only the observable facts.
- Anxious thought: The first painful interpretation.
- Feeling: Name the emotion, not the story.
- Secure reframe: A balanced sentence that is believable, not sugary.
If your reframe sounds fake, it won’t help. “Everything is perfect” won’t land. “I don’t have enough information yet” often will.
Build secure attachment reframes
A secure reframe is not a positive affirmation pasted over panic. It is a more grounded interpretation that makes room for uncertainty without collapsing into fear.
Try shifting these common thoughts:
From: “If they loved me, I wouldn’t feel this anxious.”
To: “My anxiety is telling me I need support, not that love is absent.”From: “I need an answer right now.”
To: “Urgency is part of my activation. I can pause before acting.”From: “I’m too needy.”
To: “I have attachment needs. I’m learning how to express them clearly.”From: “This feeling means something is wrong.”
To: “This feeling means my system is activated.”
The strongest reframe is the one your body can tolerate, not the one that sounds most enlightened.
Run behavioral experiments carefully
Behavioral experiments help you test a feared belief in real life. Through behavioral experiments, cognitive behavioral therapy for anxious attachment style becomes more than journaling.
The key is intention. You are not testing your partner to trap them. You are testing your own prediction and building capacity.
Experiment one: Delay the reassurance move
If you usually send a second text within minutes, wait first.
Choose a small delay that feels challenging but doable. During that pause, notice:
- What am I predicting will happen?
- What sensation am I trying to get rid of?
- Does the urge rise, peak, and soften at all?
You may discover that the panic is intense but survivable. That matters.
Experiment two: Ask directly instead of protesting
Instead of hinting, withdrawing, or becoming reactive, try one clear sentence.
For example:
“I noticed I felt anxious when we stopped texting suddenly. Could we check in later tonight?”
That kind of communication builds security better than protest behavior does.
Experiment three: Stop mind-reading and gather data
If your brain says, “They sounded cold, so they must be pulling away,” pause and look for a wider pattern.
Ask yourself:
- Is this a one-off moment or a sustained pattern?
- What else could explain this behavior?
- Have I checked in directly?
This doesn’t mean ignoring red flags. It means refusing to make a case with incomplete evidence.
A short worksheet for the moment of activation
When you're triggered, answer these four prompts:
- What happened?
- What did I make it mean?
- What do I want to do right now?
- What response would support self-respect and connection?
That final question often changes everything.
What works and what doesn’t
Some CBT practices help anxious attachment immediately. Others can turn into more rumination if used poorly.
What tends to help:
- Brief thought records: Short, specific, tied to one trigger.
- Compassionate reframes: Realistic and steady.
- Behavioral experiments: Small, repeatable, grounded in self-observation.
- Clear communication: Naming needs without accusation.
What usually backfires:
- Overanalyzing every interaction: That’s rumination wearing a therapeutic disguise.
- Using reframes to suppress hurt: You still need to feel what you feel.
- Testing your partner constantly: That increases instability.
- Waiting until you’re flooded: Practice when mildly activated too.
If you’d like to include a teaching video here from the @SecurelyLoved channel, this is a good spot for a walkthrough of a thought record in a real relationship trigger.
A real-world example
Someone I’ve worked with used to spiral whenever her partner said, “I’ll call you later,” and then called later than expected. Her old pattern was checking the time, building resentment, then sending a sharp text to cover fear with anger.
Her thought record revealed the belief underneath: “If I’m not kept in mind consistently, I don’t matter.”
That’s the kind of sentence CBT can work with.
Once she could name it, she stopped arguing with surface thoughts and started challenging the deeper assumption. Her reframe became: “A delay can be disappointing without meaning I’m forgotten.” From there, she practiced waiting, grounding, and then speaking openly rather than reacting defensively.
That is real progress. Not perfection. Not never getting triggered. A different response.
Beyond Thoughts: Calming Your Anxious Nervous System
There is a moment in attachment activation when thought work stops being enough.
You may know the secure reframe. You may even believe it intellectually. But your hands are shaking, your jaw is tight, and your body is braced for impact. That’s not the time to force more analysis. That’s the time to regulate.

Longer-term change in attachment security appears to involve more than symptom control. One summary notes that, within 6 months to 1 year of consistent CBT engagement, people often develop more secure patterns, with improvements in anxiety sensitivity and avoidance behaviors preceding changes in attachment representations in this review of cognitive behavioral therapy for anxious attachment style.
Why your body reacts so fast
Attachment patterns live in the nervous system, not just in your beliefs.
That’s why you can understand your pattern and still feel hijacked by it. Your body may register distance, ambiguity, or a shift in tone as danger long before your thinking brain catches up.
The idea of a window of tolerance proves helpful. When you’re inside that window, you can think, feel, reflect, and respond. When anxious attachment pushes you outside it, you move into panic, urgency, or collapse.
If you want a fuller grounding in this body-based lens, this explanation of what is nervous system regulation gives a helpful overview.
Three somatic tools that pair well with CBT
These practices are simple on purpose. In a trigger, simple is what works.
Orienting to the present
When your body is acting like danger is here, gently show it where you are.
Look around the room slowly. Let your eyes land on objects, edges, colors, light, and distance. Don’t rush it.
Say to yourself:
- I’m in my bedroom.
- The door is closed.
- The lamp is on.
- The rain is outside.
- I’m here right now.
Orienting helps interrupt the body’s reflex to lock onto the imagined threat.
Hand-on-heart breathing
Put one hand on your chest and one on your upper belly if that feels okay. Breathe in naturally. Exhale a little longer than you inhale, without straining.
As you do this, try one sentence:
“I’m activated, and I can stay with myself.”
This isn’t about instantly calming down. It’s about sending a cue of support inward.
When your nervous system feels alone, your thoughts get louder. When your body feels accompanied, your thoughts often soften.
Five-senses grounding
Use this when your mind is racing and you need structure.
Notice:
- Five things you see
- Four things you feel
- Three things you hear
- Two things you smell
- One thing you taste
This works because it moves attention from imagined future loss back to the current environment.
How to combine CBT and body regulation
Try this sequence when you're triggered:
| Step | Focus |
|---|---|
| 1 | Name the trigger in one sentence |
| 2 | Regulate your body with orienting or breathing |
| 3 | Write the anxious thought |
| 4 | Create a secure reframe |
| 5 | Choose one grounded action |
That order matters. If you try to challenge a thought while your body is in full alarm, the reframe may bounce right off.
What embodied safety looks like
Embodied safety is not the absence of longing, grief, or vulnerability.
It’s the growing ability to feel activated without immediately abandoning yourself. It’s being able to say, “This is hard,” without making the feeling mean you’re about to be left. It’s choosing a regulated pause over a frantic move.
That’s often the missing piece in traditional cognitive work. Your thoughts need support from your body. Your body needs support from your thoughts. Together, they create enough steadiness for secure attachment to take root.
Making It Stick: Navigating Pitfalls and Setbacks
People often assume that if CBT is working, triggers should stop happening quickly.
That assumption causes a lot of unnecessary shame.
Healing anxious attachment usually looks less dramatic than people expect. You may still get activated. The difference is that you recover faster, act with more awareness, and create less damage while upset.
The urge to quit is common
Across anxiety-related disorders, CBT has a 22% dropout rate, and nonadherence for exposure-based work can range from 31% to 65%, according to this overview of cognitive behavioral therapy and anxious attachment. The same source highlights the importance of support and strong intervention in the first 4 to 6 weeks.
That matters because many people decide “this isn’t working” right when the work becomes emotionally real.
Common pitfalls that slow progress
Using CBT to argue with your feelings
A secure response doesn’t say, “I shouldn’t feel hurt.”
It says, “I feel hurt, and I’m going to respond with care instead of panic.”
If you use CBT as a way to suppress sadness, anger, or grief, your body usually protests louder later.
Turning thought work into rumination
A useful thought record is short and clarifying. An unhelpful one becomes a courtroom where you retry the relationship all night.
If you notice yourself getting more activated as you write, stop. Regulate first. Return later.
Expecting a straight line
Setbacks don’t erase progress. They reveal where your system still needs support.
I often tell clients to measure healing by questions like these:
- Recovery time: Am I coming back to center sooner?
- Behavior change: Am I reducing protest behaviors?
- Self-relationship: Am I staying kinder to myself when I’m triggered?
- Communication: Am I saying what I need more directly?
A setback is often old learning under stress, not proof that nothing has changed.
What helps when you feel discouraged
Try a rupture-and-repair mindset with yourself.
If you had a hard week, sent the extra texts, spiraled, or shut down, pause before turning that into an identity statement. Don’t jump to “I’ll always be this way.”
Instead:
- Name what triggered you.
- Identify what support was missing.
- Repair with yourself before repairing with anyone else.
- Return to one tool, not all the tools.
That last point is important. Overhauling everything when you feel shaky usually backfires. Pick one steadying practice and use it consistently.
What actually builds traction
Progress sticks when the work is realistic.
That usually means:
- Smaller experiments: Not the hardest trigger first.
- Predictable practice: Using tools outside crisis moments.
- Relational support: A trusted person, therapist, or structured container.
- Self-compassion: Firm, honest, and non-shaming.
People rarely fail CBT because they are incapable of change. More often, they try to do it while flooded, isolated, or perfectionistic. That is a setup for discouragement, not healing.
When Self-Help Is Not Enough: Your Path Forward
Self-help can take you far. Sometimes it takes you to the edge of what you can hold alone.
If your anxious attachment is rooted in significant trauma, repeated relational injury, emotional neglect, or patterns that feel bigger than your coping capacity, support matters. Not because you’re broken. Because some attachment wounds need to be healed in relationship, with guidance that is careful enough for your nervous system.
Signs it may be time for professional help
You don’t need to be in crisis to benefit from therapy. A few signs that self-help may not be enough:
- You understand the tools but can’t use them when activated.
- Your relationships keep following the same painful script.
- You swing between panic and shutdown.
- You aren’t sure whether what you’re dealing with is anxious attachment, trauma activation, or another anxiety pattern.
- You use CBT exercises, but they turn into self-criticism or overanalysis.
A therapist can help you sort out what belongs to cognition, what belongs to the body, and what belongs to your attachment history.
Why individual tailoring matters
Not everyone responds to CBT in the same way. Research shows that baseline attachment dimensions affect treatment response, and that clients with dismissing or avoidant attachment patterns may do better with CBT that includes more interpersonal and emotional processing, as discussed in this study on attachment dimensions and CBT response.
That’s one reason generic advice often falls short.
If you’re weighing next steps, this reflection on the limitations of cognitive behavioral therapy may help you see where CBT works well and where an integrated approach becomes important.
What to look for in a therapist
Look for someone who understands:
- Attachment dynamics: Not just anxiety symptoms.
- Trauma-informed care: So overwhelm is handled skillfully.
- Somatic regulation: So your body isn’t left out of the work.
- Relational nuance: Because not every “trigger” is irrational, and not every relationship is safe.
The right support won’t force you to choose between practical tools and deep healing. It should offer both.
If you’re ready for support that blends attachment-focused therapy with nervous system regulation, Securely Loved offers a gentle place to begin. Bev Mitelman’s practice is designed for adults who feel stuck in repeating relationship patterns and want more than insight alone. You can book a free 15-minute connection call to explore fit, ask questions, and talk through what support might look like for you.
