
Hypervigilance in Relationships: Why You Feel On Edge
You’re lying in bed next to someone you care about. The evening was ordinary. Maybe even nice. Then they got a little quiet.
Now your mind is racing.
You replay dinner. You reread their last text. You notice they took a little longer than usual to answer. A knot forms in your stomach and your body starts acting like a breakup is already happening.
By morning, you’re not just uneasy. You’re bracing. You want to ask, “Are we okay?” but part of you also feels embarrassed for needing to ask at all.
If that experience feels painfully familiar, you’re not broken, needy, or “too much.” You may be dealing with hypervigilance in relationships.
This pattern can make love feel like something you have to monitor instead of something you get to receive. It can turn a delayed reply, a change in tone, or a distracted look into a full-body alarm. And if you’ve lived through inconsistent care, betrayal, emotional unpredictability, or attachment trauma, that alarm makes sense.
Hypervigilance is a protection strategy. It just stops helping when your nervous system keeps reacting to old danger inside present-day relationships.
That Feeling Your Relationship Is About to End
A client once described it this way. “Nothing bad has happened, but I feel like I need to prepare.”
That’s often how hypervigilance shows up. Not as dramatic panic at first, but as a constant inner readiness for loss. Your partner says, “I’m tired,” and your body hears, “I’m done with you.” They seem distracted after work, and your mind starts building a case that you’ve done something wrong.
When neutral moments feel dangerous
The hardest part is that the trigger is often small.
- A slower text reply can feel like withdrawal.
- A quiet car ride can feel like punishment.
- A shorter-than-usual answer can feel like rejection.
- A normal need for space can feel like abandonment.
You may know logically that none of this proves the relationship is ending. But your body isn’t responding to logic in that moment. It’s responding to threat.
You can be in a loving relationship and still feel chronically unsafe inside it.
That inner split confuses a lot of people. They tell themselves, “I shouldn’t feel this way,” which adds shame on top of fear.
Why this feels so exhausting
Hypervigilance keeps your system on guard. You don’t just notice your partner. You track them. You scan for clues. You try to predict shifts before they happen.
That takes enormous energy.
It also creates a painful cycle. The more distressed you feel, the more reassurance you seek. The more reassurance you seek, the more ashamed or dependent you may feel. Then your body reads that shame as another sign that something is wrong.
If this is your pattern, you don’t need more self-criticism. You need a clearer understanding of what your system is trying to do, and better ways to help it stand down.
What Is Relationship Hypervigilance Really
Relationship hypervigilance is a state of persistent threat-scanning in close connection. Your mind and body start watching for signs of rejection, anger, withdrawal, betrayal, or abandonment, even when the evidence is thin or unclear.
A useful way to understand it is this. Your emotional smoke alarm is too sensitive.
A healthy smoke alarm should go off for an actual fire. A hypervigilant one goes off for burnt toast, steam from the shower, and someone lighting a candle three rooms away. The alarm is trying to protect you. It’s just miscalibrated.
It isn’t the same as intuition
People often ask whether they’re sensing something real or spiraling.
Healthy intuition usually feels clearer, steadier, and less urgent. Hypervigilance feels fast, physical, repetitive, and hard to turn off. Intuition can leave room for curiosity. Hypervigilance pushes you toward certainty, usually worst-case certainty.
What it tends to look like day to day
You might notice that you:
- Scan tone and facial expressions for signs that something is off
- Replay conversations to look for mistakes
- Assume negative intent before asking questions
- Need repeated reassurance but struggle to believe it
- Feel suspicious of calm because peace doesn’t feel trustworthy
- Overfunction in the relationship to prevent disconnection
None of that means you’re dramatic. It means your nervous system has learned that closeness can change quickly, so it keeps watch.
Hypervigilance vs Healthy Attentiveness
| Behavior/Mindset | Hypervigilant Response (Threat-Based) | Healthy Attentiveness (Connection-Based) |
|---|---|---|
| Partner seems quiet | “They’re upset with me.” | “They seem quiet. I’ll check in.” |
| Delayed text | “They’re pulling away.” | “They may be busy. I can wait and see.” |
| Conflict | “This could mean abandonment.” | “This is uncomfortable, but we can talk through it.” |
| Need for reassurance | Asking repeatedly, then doubting the answer | Asking directly, then taking in the response |
| Reading body language | Searching for proof of danger | Noticing cues with curiosity, not certainty |
| Sense of responsibility | Feeling you must manage the bond at all times | Trusting that both people help maintain connection |
| Calm periods | Feeling uneasy, waiting for the other shoe to drop | Letting ease feel like ease |
A body response, not a personality flaw
This matters. Hypervigilance isn’t just a thinking habit.
It’s often a nervous system pattern. Your body starts mobilizing before your conscious mind has fully formed a story. That’s why you may feel a tight chest, clenched jaw, racing thoughts, or a sinking feeling before you can even explain what’s wrong.
Practical rule: If your body reacts first and your mind scrambles to justify it second, you’re likely dealing with a threat response, not a character defect.
That distinction changes the work. If you treat hypervigilance as a moral failure, you’ll keep trying to think your way out of it. If you understand it as a protection strategy, you can start responding with regulation, clarity, and support.
The Roots of Hypervigilance in Trauma and Attachment
People don’t usually become hypervigilant in relationships for no reason. This pattern is often learned in environments where connection felt inconsistent, confusing, or emotionally unsafe.
If you had to read the room growing up, you probably got very good at it. If a caregiver’s mood shifted without warning, if affection felt conditional, or if closeness also carried stress, your nervous system adapted. It learned that paying close attention might prevent pain.
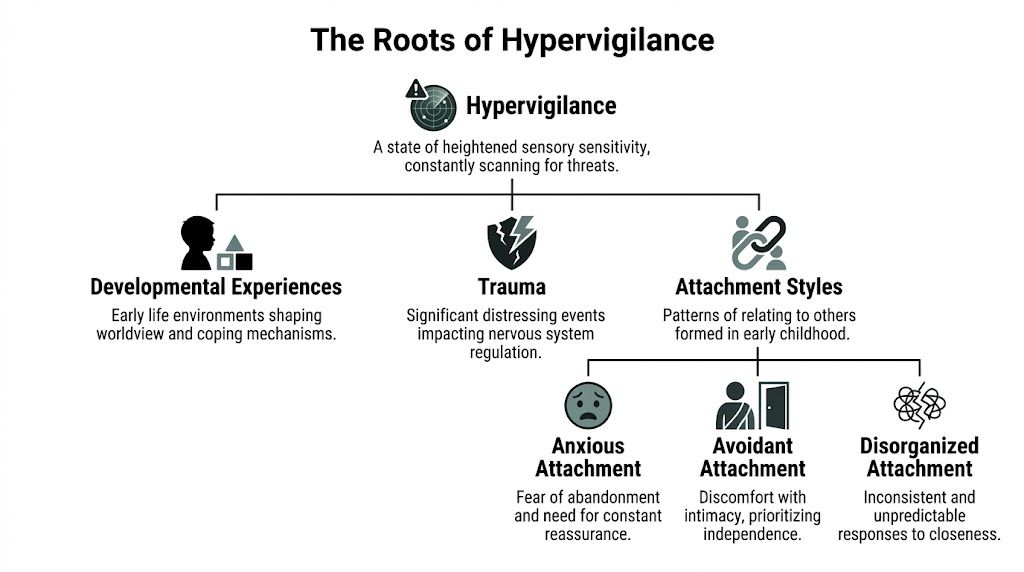
How attachment shapes what you scan for
Different attachment patterns often organize hypervigilance in different ways.
- Anxious attachment often scans for distance. You notice delayed responses, changes in tone, and signs of fading interest.
- Avoidant attachment often scans for intrusion. You track demands, expectations, and signals that someone wants too much closeness.
- Disorganized attachment often scans for both. You want connection, but your body also braces against it.
That’s why two people can both be hypervigilant and look very different from the outside. One pursues. One withdraws. Both are protecting against pain.
Early adaptation can become a present-day trap
Children who grow up with inconsistent emotional attunement often become adults who overread relationships. They may overexplain, self-silence, test loyalty, or rehearse difficult conversations in their heads before anything has happened.
Those habits are intelligent adaptations. But in adult intimacy, they can create a life where love feels tense even when it’s available.
A trauma-informed, attachment-based approach can help people understand these patterns at the root, not just manage them at the surface. Work like attachment trauma therapy focuses on the deeper wiring underneath the reaction.
The research supports this pathway
A 2023 study found that hypervigilance plays a mediating role between post-traumatic stress and marital insecurity. The model showed a significant direct effect of post-traumatic stress on hypervigilance (β = .58) and of hypervigilance on marital insecurity (β = .53), which supports the idea that trauma symptoms heighten threat scanning and that scanning contributes to relational distress, according to the Journal of Research in Psychology and Counseling Techniques study.
That matters because many people blame themselves for what is a patterned response.
When someone says, “I know I’m overreacting, but I can’t stop,” I don’t hear dysfunction first. I hear a nervous system doing exactly what it learned to do.
Healing usually starts when you stop asking, “Why am I like this?” and begin asking, “What taught my body that closeness needed this much monitoring?”
How Hypervigilance Secretly Erodes Intimacy
Hypervigilance often shows up as devotion at first. You care a great deal. You notice everything. You try to stay connected.
But over time, the same strategies that aim to create safety can slowly wear down the relationship.

The cycle most people miss
A common pattern looks like this:
- You detect a cue. A pause, a tone shift, a short text.
- Your body goes on alert. Anxiety rises fast.
- You seek certainty. Reassurance, checking, questioning, pulling away first.
- Your partner feels pressure or confusion.
- Connection becomes strained, which then seems to confirm your fear.
That’s why hypervigilance in relationships feels so cruel. The protection can accidentally help create the very disconnection you’re trying to prevent.
Real-world examples
This pattern rarely looks dramatic from the outside. It often looks ordinary.
- Text analysis. You reread “Okay” five times to decide whether it’s irritated, cold, or fine.
- Repeated checking. You ask, “Are we okay?” not because you want attention, but because your body wants relief.
- Preemptive shutdown. You go quiet before they can disappoint you.
- Mind-reading attempts. You assume what they feel instead of asking.
- Overfunctioning. You try to be low-maintenance, useful, easy, and endlessly understanding so they won’t leave.
Each move makes sense. None of them create durable safety.
Why the brain and body stay stuck
Neuroscience points to amygdala hyperactivity as part of hypervigilance, keeping the body in a survival state where even positive experiences can feel unsafe. The same source notes that a longitudinal study of 4,796 married couples found a wife’s daily anxiety significantly correlated with both partners’ perceived relationship quality, showing that this kind of distress affects the relationship in both directions, as described by the CPTSD Foundation article on hypervigilance and relationships.
When your system is mobilized like that, vulnerability gets harder. Playfulness drops. Ease drops. You may still show up physically, but emotionally you’re managing risk.
What intimacy actually needs
Intimacy needs room.
It needs the ability to ask instead of assume. To hear reassurance and let some of it land. To tolerate a little uncertainty without organizing your whole inner world around it.
If this dynamic is part of an anxious-avoidant loop in your relationship, hearing it explained visually can help. This video from Bev Mitelman explores the pattern in a practical way:
The goal isn’t to become less sensitive. It’s to become less governed by threat.
That shift lets sensitivity become discernment instead of surveillance.
Practical Ways to Calm a Hypervigilant Nervous System
Insight helps. Regulation changes things.
If hypervigilance lives in your body, then healing has to include your body too. You don’t need to force yourself to stop caring. You need practices that help your system recognize safety again.

Start by mapping your state
A simple nervous system map can help.
- Green zone means you feel present enough to connect, think, and respond.
- Yellow zone often feels like anxiety, urgency, irritation, or overanalysis.
- Red zone can feel numb, shut down, disconnected, or hopeless.
You don’t need to map this perfectly. You just want to start noticing, “What state am I in right now?” before acting from it.
If you want a deeper explanation of this process, nervous system regulation is a useful framework for understanding why your body reacts before your mind catches up.
Three practices that work in real life
Ground in the present
This is useful when your mind is racing ahead.
Try this:
- Name what you see. Pick a few objects in the room and describe them plainly.
- Feel your support. Notice your feet on the floor or your back against a chair.
- Lengthen the exhale. Don’t force a deep breath. Let the out-breath get a little longer.
This helps orient your system to the current moment instead of the feared scenario.
Use pendulation
Pendulation means gently moving between activation and something more neutral or settling. You’re not trying to suppress the alarm. You’re helping your body learn it can move in and out of intensity.
Try it this way:
- Notice the activated sensation. Maybe it’s a tight chest.
- Stay with it briefly, only as much as feels manageable.
- Shift attention to something steadier. A warm mug, your feet, a safe sound.
- Move back and forth slowly.
This approach matters because somatic hypervigilance stems from a dysregulated autonomic response, and trauma-informed protocols using pendulation have been reported to achieve 40% symptom reduction in 8 to 12 weeks, benchmarked by reduced reassurance-seeking and measurable heart rate variability changes, according to the Compass Healing Project article on somatic hypervigilance.
Track glimmers
People often focus only on triggers. Glimmers are the small cues of safety that help retrain the system.
Look for:
- A softening in your chest when someone speaks kindly
- A moment of ease in the shower, on a walk, or in sunlight
- A settled breath after your partner responds clearly
- A sense of grounding when you hear a familiar voice
These moments may seem minor. They matter because your nervous system changes through repetition.
What doesn’t work well on its own
Some approaches help less than people hope.
- Arguing with yourself when you’re already flooded often backfires.
- Demanding instant certainty trains the cycle instead of calming it.
- Endless self-analysis can become another form of scanning.
- Traditional insight-only work may leave the body pattern untouched.
That doesn’t mean talking is useless. It means insight works best when paired with embodied practice.
Build a pause between trigger and action
One of the most healing micro-skills is this question:
“What does my body need before I decide what this means?”
That pause changes a lot. It helps you stop treating activation as evidence.
With support, people also use structured approaches such as HRV biofeedback, body-based therapy, and attachment-focused work. Securely Loved is one example of a practice that integrates attachment history with nervous system regulation for adults who feel stuck in these patterns.
Small repeated practices usually work better than intense occasional ones. A five-minute regulation habit done regularly can change more than a long exercise you only try when things are falling apart.
The Underdiscussed Link to Midlife and Menopause
Many women hit midlife and feel blindsided by relationship anxiety that suddenly seems louder, faster, and harder to regulate. They often tell themselves they should be past this by now.
They’re not failing. Their nervous system may be under more strain.
It isn’t “just hormones”
Hormonal shifts can amplify a preexisting trauma pattern. That’s different from saying the whole experience is caused by hormones alone.
An underserved angle in this conversation is the link between hypervigilance and midlife hormonal transition. Fluctuating estrogen can intensify nervous system hyperarousal, and emerging post-April 2025 data noted a 25% rise in perimenopausal women reporting attachment-related anxiety linked to hypervigilance, highlighting a need for more integrated care, as described in this HealthMatch overview of hypervigilance in relationships.
For the woman who has always been high-functioning, this can feel especially disorienting. You may still excel at work, manage a household, and show up for everyone else. But inside your relationships, your tolerance for ambiguity drops. Small shifts hit harder. Recovery takes longer.
What this can look like in real life
You may notice:
- More sensitivity to distance from a partner, even in a stable relationship
- Less buffering capacity after poor sleep or stress
- A stronger startle into fear during normal conflict
- Greater difficulty settling after reassurance
That doesn’t mean your relationship has suddenly become unsafe. It may mean your body has less margin.
Integrated care matters
Emotional and physical assessment need to work together.
If you’re trying to understand whether hormonal changes may be part of the picture, a resource on a menopause blood test can help you think through what medical evaluation may and may not clarify. It’s not a replacement for trauma work, but it can be part of a more complete picture.
For many women, the missing piece is understanding how midlife biology and attachment injury interact. Support that speaks to both can be far more relieving than being told to “just manage stress” or dismissing it all as moodiness. This is also why focused education on menopause and anxiety symptoms can be so useful.
Midlife doesn’t create attachment wounds. It can turn up the volume on the ones that never got fully addressed.
That framing often brings a lot of relief. It replaces shame with context.
Finding Professional Support That Truly Works
When hypervigilance has been running your relationships for years, self-help alone may not be enough. Support matters. The type of support matters even more.
Many people have already tried traditional talk therapy before they find what works. They understood their story. They could name their attachment style. They still felt hijacked by the same reactions.
What to look for in a therapist
A useful fit usually includes these elements:
- Trauma-informed care so the therapist understands protective responses instead of pathologizing them
- Attachment-focused work so your relationship patterns are part of the treatment, not an afterthought
- Somatic or body-based tools so your nervous system gets addressed directly
- Pacing and attunement so you’re not pushed into insight faster than your body can integrate
If a therapist only asks you to challenge thoughts without helping you notice activation, settle your body, and work with relational triggers, progress can feel limited.
Why insight alone often falls short
Hypervigilance isn’t just a belief. It’s a body expectation.
That’s why someone can say, “I know my partner loves me,” and still feel panicked when they don’t text back. The goal of therapy isn’t to make you think nicer thoughts while your body remains in alarm. The goal is to help your body stop treating closeness like an unstable environment.
If your relationship stress is tangled with separation, breakup, or divorce concerns, practical reading on professional support and coping strategies related to relationship stress can also be useful alongside therapy.
A good therapist helps you do more than vent
A strong process usually helps you:
- notice your triggers earlier
- understand the attachment meaning you assign to them
- regulate before reacting
- practice new relational responses
- build a steadier sense of internal safety
This video from Bev Mitelman offers guidance on finding the right kind of support for attachment trauma:
The right support won’t shame your sensitivity. It will help you understand it, work with it, and gradually need less protection from it.
Your Questions on Relationship Hypervigilance Answered
How do I know if it’s hypervigilance or intuition
Look at the quality of the experience.
Intuition usually feels more grounded and specific. Hypervigilance tends to feel urgent, repetitive, body-heavy, and organized around proving danger. Intuition can coexist with calm. Hypervigilance usually pulls you away from it.
A simple check is to ask yourself whether you can stay curious. If your mind is demanding immediate certainty and your body feels braced, that’s usually a clue that a threat response is active.
Can hypervigilance happen in a healthy relationship
Yes. Often.
A healthy relationship can expose an old wound because steadiness gives you fewer obvious problems to focus on. Then your system starts scanning subtler cues. That doesn’t mean the relationship is the cause. It may be the place where your unresolved fear becomes visible.
Should I tell my partner about this
Usually yes, if they’re emotionally safe enough to hear it.
Keep it simple. Try language like, “When connection feels uncertain, my nervous system can go on alert. I’m working on it, and it helps when we communicate clearly.” That’s more effective than delivering a long apology or expecting them to decode your reactions.
What should I do in the moment instead of asking for reassurance again
Pause before you reach out.
Try to identify what state your body is in. Ground first. Delay action briefly if you can. Then ask yourself whether you need information, comfort, or regulation. Sometimes the urge for reassurance is really a need for settling.
Can this pattern actually change
Yes, but it usually changes through repeated lived experience, not one big insight.
You’re helping your body learn that closeness can be tolerated without constant monitoring. That takes practice, grief, patience, and often skilled support. It’s slow work for many people, but it is absolutely possible.
Is my attachment style permanent
No.
Your history shapes you, but it doesn’t lock you in place. Attachment patterns can become more secure when you build internal safety, choose healthier relational experiences, and work with the nervous system responses underneath the pattern.
If this article felt uncomfortably familiar, that’s often the first sign you’re finally naming the right thing. Secure, grounded love doesn’t come from monitoring harder. It comes from helping your body feel safer in connection. Securely Loved offers attachment-focused, trauma-informed support for adults who are ready to understand their patterns, regulate their nervous system, and build more secure relationships.
