
Attachment Trauma Therapy: A Guide to Healing
Some people arrive at attachment trauma therapy feeling confused by how capable they are everywhere except in love. They manage teams, care for aging parents, keep up with deadlines, and look composed from the outside. Then a partner pulls back, a text goes unanswered, or intimacy starts to deepen, and suddenly their whole system spirals.
For one person, that spiral looks like checking their phone every few minutes and replaying conversations late into the night. For another, it looks like going numb, losing interest, and deciding they do not need anyone anyway. Some live in the exhausting middle, craving closeness one day and wanting to disappear the next.
If that sounds familiar, the problem is probably not that you are too needy, too much, too guarded, or bad at relationships. Often, these patterns grow out of attachment trauma, the early relational injuries that teach your body and mind what to expect from closeness. Sometimes that trauma is obvious. Sometimes it is the slow ache of inconsistent emotional attunement, criticism, distance, or having to become the responsible one too early.
That is why insight alone so often falls short. You may already understand your pattern intellectually and still feel hijacked in real time. Attachment trauma therapy works at a deeper level. It helps you understand your relational blueprint, notice how your nervous system reacts to connection, and build the kind of internal safety that makes secure relationships possible.
Healing does not mean becoming perfect, calm, or endlessly available. It means becoming more anchored in yourself, less driven by old survival strategies, and more able to receive love without losing your footing. That path is real, and it is learnable.
Introduction
You might be reading this after another disappointing relationship, or in the middle of one that leaves you second-guessing yourself. Maybe you keep choosing emotionally unavailable partners. Maybe you have a loving partner and still feel braced for abandonment. Maybe you shut down the moment someone gets too close, then feel lonely when they stop trying.
High-functioning adults often blame themselves for this. They say things like, “I know better,” or “Why do I keep doing this?” Shame fills in the gaps where understanding should be.
Attachment trauma therapy offers a different lens. It treats these reactions as adaptations, not character flaws. What looks irrational in the present often made complete sense in an earlier environment where love felt inconsistent, overwhelming, conditional, or unsafe.
A client might say, “Nothing terrible happened in my childhood, so why am I like this?” That question matters. Attachment wounds do not always come from a single dramatic event. They can form when a child regularly has to suppress needs, read the room to stay connected, or handle distress without enough comfort.
When the pattern makes sense
If you learned that closeness could disappear without warning, your adult nervous system may scan for signs of rejection. If vulnerability led to disappointment, your body may protect you by withdrawing before anyone can matter too much.
That is why attachment trauma therapy is not about blaming parents or excavating the past for its own sake. It is about understanding the link between early relationships and present-day survival patterns.
Key takeaway: Your relationship pattern is not your identity. It is a strategy your system learned to protect connection, dignity, or survival.
What healing starts to look like
As therapy unfolds, people often become less reactive, more discerning, and more able to stay present during discomfort. They learn how to pause before pursuing, soften before shutting down, and recognize the difference between actual danger and old alarm.
That shift can feel small at first. You answer a text later without panicking. You name a need without apologizing for having one. You notice your body bracing and choose to stay with yourself instead of abandoning yourself. Secure connection begins in these moments.
Understanding Your Attachment Blueprint
Attachment is your relational blueprint. It is the internal template your system built early in life about what closeness means, what to expect from other people, and what you have to do to stay connected.
That blueprint keeps shaping adult relationships until it is brought into awareness and updated through new experiences.
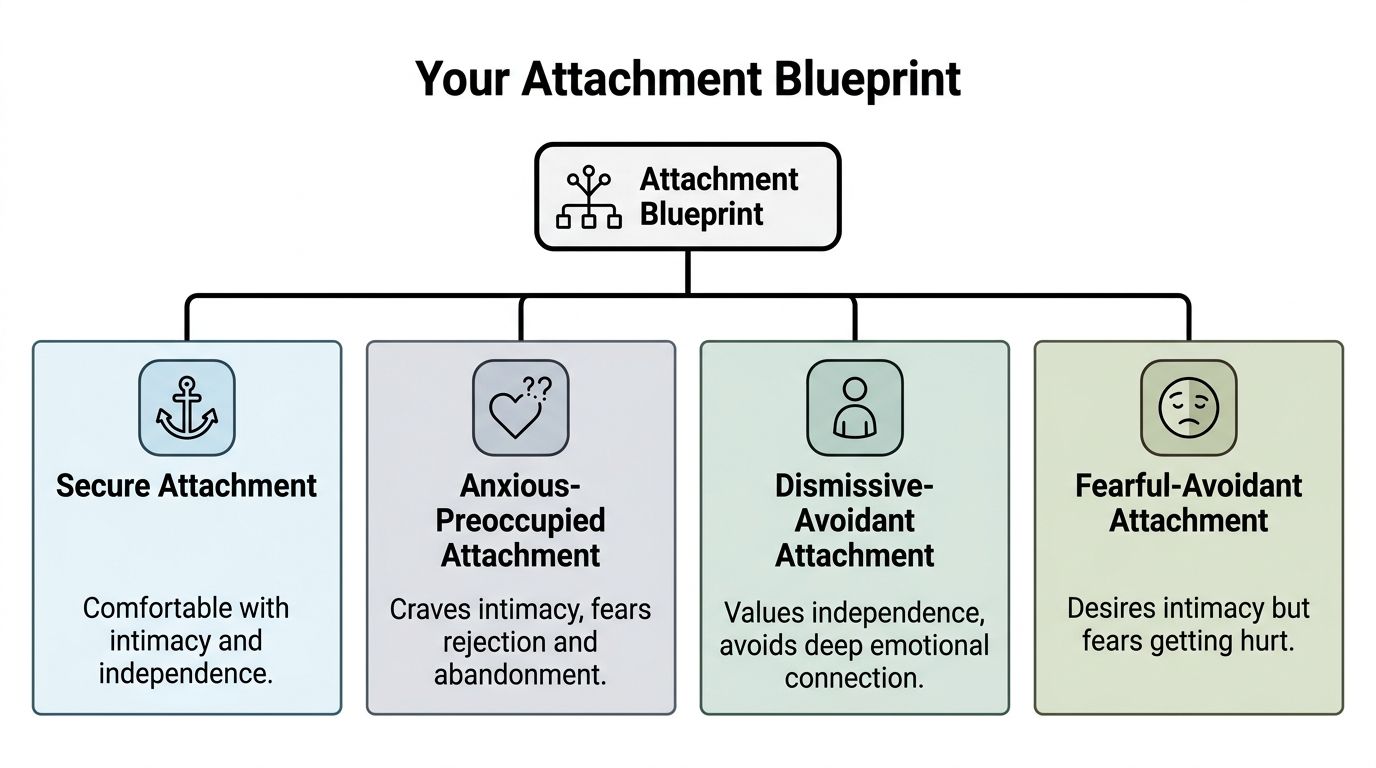
The four patterns most adults recognize
A secure attachment pattern usually feels steady. You can get close without panicking and take space without assuming the relationship is over. You trust repair is possible after conflict.
An anxious attachment pattern often feels like relational hypervigilance. You might need reassurance, read into small shifts, or feel destabilized when someone becomes less responsive. A delayed reply can feel enormous, even when part of you knows it should not.
A dismissive-avoidant attachment pattern tends to protect through distance. You may value independence so strongly that need itself feels uncomfortable. When someone wants more closeness, your instinct may be to minimize feelings, focus on logic, or create emotional space.
A fearful-avoidant or disorganized attachment pattern often carries the most inner conflict. You want love and fear it at the same time. You may move toward intimacy and then feel overwhelmed, suspicious, ashamed, or compelled to pull away.
For a fuller breakdown of these patterns, this guide on attachment style definition can help you identify what fits.
Trauma is not always loud
Many adults dismiss their own attachment wounds because they compare themselves to people with more obvious histories. That comparison keeps people stuck.
Attachment trauma can come from abuse and neglect, but it can also come from repeated emotional misattunement. A child does not need to be physically harmed to learn, “My feelings are too much,” “I have to earn love,” or “No one comes when I need comfort.”
Research helps put this in perspective. A meta-analysis reported global prevalence of emotional abuse at 36.3% and emotional neglect at 18.4%, and linked these early experiences with insecure attachment, PTSD risk, and relational difficulty in adulthood, as detailed in this Frontiers review on attachment trauma and psychopathology.
How these blueprints show up in ordinary life
You do not need to analyze your entire history to spot your pattern. Start with your lived moments:
- After conflict: Do you lean in harder, pull away, or freeze?
- When someone loves you consistently: Do you relax, doubt it, or lose interest?
- When you need support: Can you ask directly, or do you hint, overexplain, or go silent?
- When intimacy deepens: Do you feel grounded, trapped, suspicious, or emotionally flooded?
A useful question is not “What is wrong with me?” It is “What did my system learn about closeness?”
Your blueprint is learned, not fixed
Attachment styles describe tendencies, not life sentences. They are patterns of adaptation. They can change when you experience enough safety, consistency, repair, and embodied practice.
That matters because many adults already know their attachment style, but they use that knowledge like a label instead of a doorway. Naming the pattern is only the first step. Healing begins when you learn what the pattern is trying to protect.
A partner forgetting to text back is not just a missed message in this framework. For an anxious system, it may register as danger. For an avoidant system, a request for deeper connection may register as pressure. For a disorganized system, love itself may activate both longing and alarm.
Once you understand the blueprint, your reactions start to make sense. And when they make sense, they become workable.
Practical reframe: Stop asking whether your reaction is “too much.” Ask what fear, expectation, or old lesson the reaction is organized around.
If you want to add a video here, an explainer from @SecurelyLoved (Bev Mitelman) on the attachment styles would fit naturally in this section.
How Attachment Trauma Lives in Your Nervous System
People often come to therapy saying, “I understand my childhood. Why am I still reacting like this?” The short answer is that attachment trauma is not only stored as a story. It is also stored as a state.
Your body learned what connection feels like before it had language to explain it.
The safety ladder
A simple way to understand this is through a safety ladder.
At the top is a safe and social state. You feel more present, flexible, connected, and able to think clearly. You can take in nuance. You can hear feedback without collapsing or attacking.
In the middle is fight or flight. Your system mobilizes. You may become anxious, restless, irritable, fixated, persuasive, controlling, or desperate to resolve things immediately.
At the bottom is shutdown or freeze. You may feel numb, flat, foggy, detached, hopeless, or emotionally unavailable. This is not laziness or indifference. It is a protective state.
How this plays out in relationships
A partner says, “We need to talk.” One person goes straight into panic and starts overexplaining, apologizing, or trying to secure reassurance. Another person suddenly feels tired, distant, or blank and cannot access words. Someone else gets sharp and defensive because their body is preparing for threat.
These are nervous system responses before they are relationship strategies.
That is why cognitive insight is helpful but incomplete. If your body is already in alarm, telling yourself to calm down may not land. Attachment trauma therapy helps you notice state shifts earlier and build a bridge back to regulation.
For a deeper look at this process, this page on what nervous system regulation is gives a clear foundation.
Signs your body is carrying the wound
Attachment trauma often shows up in very ordinary moments:
| Experience | What it may feel like in the body |
|---|---|
| Waiting for a reply | Tight chest, racing thoughts, urge to check |
| Someone gets emotionally close | Restlessness, heat, pressure, urge to escape |
| Conflict at home | Shaking, mental fog, collapse, going blank |
| Healthy consistency | Suspicion, boredom, discomfort, disbelief |
None of these reactions mean you are broken. They mean your system learned to prioritize protection.
Why body-up healing matters
A purely top-down approach often leaves people frustrated. They can explain their pattern beautifully and still feel hijacked by it on date night, during conflict, or after a breakup.
Body-up work gives the nervous system a different experience. That may include noticing tension, tracking activation, orienting to the room, lengthening the exhale, feeling your feet on the floor, or learning how to stay with a hard feeling without escalating it.
Therapy tip: If your reaction feels faster than thought, work with the body first. Insight tends to land better once the nervous system is less mobilized or shut down.
This is also why progress can feel strange at first. Regulation does not always feel blissful. Sometimes it feels unfamiliar. If your system grew up around inconsistency, calm may initially read as dull, suspicious, or unsafe.
That does not mean healing is failing. It often means your body is learning a new baseline.
If you want a video in this section, an @SecurelyLoved (Bev Mitelman) video on nervous system regulation basics would be the right fit.
Your Healing Journey What to Expect in Therapy
Many individuals feel some combination of hope and caution before starting attachment trauma therapy. They want relief, but they do not want to be overwhelmed. That caution makes sense.
Good therapy does not force depth before safety exists.

The first phase is safety, not excavation
In the beginning, therapy often focuses less on retelling your hardest memories and more on building enough steadiness to stay with yourself.
That can include noticing when you leave your body, understanding your triggers, identifying relational patterns, and learning simple regulation tools. You might talk, but you may also pause to notice your breathing, jaw tension, stomach drop, or impulse to appease.
A lot of adults are surprised by this. They expect therapy to be mostly verbal analysis. In attachment trauma work, the therapeutic relationship itself matters. The way your therapist responds, paces, and repairs small misattunements becomes part of the healing.
A typical session feels more active than people expect
One week you may explore a conflict with your partner and realize your panic started before the argument itself. Another week you may track what happened in your body when someone disappointed you.
Sessions often include a mix of:
- Reflection: Making sense of a recent rupture, dating pattern, or family dynamic.
- Regulation practice: Grounding, orienting, slowing the pace, or learning how to come back from activation.
- Parts awareness: Noticing the side of you that pursues, the side that shuts down, and the side that feels ashamed of both.
- Relational repair: Experimenting with new ways to express needs, boundaries, or uncertainty.
Maria’s pattern
Consider “Maria,” a composite example drawn from common clinical patterns. She was successful at work, thoughtful with friends, and chronically anxious in romantic relationships. If a partner became quiet, she lost sleep, overanalyzed every detail, and either protested for reassurance or pretended she needed nothing.
In therapy, Maria initially wanted strategies to stop overthinking. Those helped some. The deeper shift came when she noticed that her body reacted to distance as if she were about to be left alone emotionally, not just inconvenienced by a partner’s mood.
Once she could track that activation, the work changed. She learned to pause before texting repeatedly, name what she was feeling, and ask for connection directly instead of escalating or collapsing. She also became more discerning. She stopped calling unpredictability “chemistry.”
That is often what healing looks like. Not becoming detached, but becoming more anchored.
Structured methods can support this process
Some therapists integrate structured approaches such as Trauma-Focused CBT within attachment work. In that model, treatment often moves through psychoeducation, skill-building, and trauma narration, and pre- and post-treatment assessments described in this overview of attachment trauma therapy and TF-CBT phases report a 60% shift toward secure attachment scores and a 50% decrease in relationship sabotage behaviors at 6-month follow-up.
Those numbers matter, but the lived experience matters too. People often describe progress in practical terms:
- They stop interpreting every boundary as rejection.
- They recover more quickly after conflict.
- They can feel sadness without spiraling into shame.
- They choose partners who feel steady, not just familiar.
What works: Slow pacing, body awareness, co-regulation, and honest naming of patterns.
What does not work well: Flooding yourself with memories before you have tools, or treating attachment wounds like a simple mindset issue.
Therapy includes practice outside the room
Healing does not happen only during the session hour. It grows through repetition.
You may practice pausing before sending the fourth text. You may notice your shoulders rise when your partner is late. You may track the difference between a current disappointment and an old abandonment alarm. These moments are not detours from the work. They are the work.
Over time, your system starts to trust that closeness does not always equal danger, and distance does not always equal loss. That trust is built through experience, not force.
Evidence-Informed Therapies That Create Change
Attachment trauma therapy is not one single method. It is better understood as a clinical orientation with a toolkit. Different therapies reach different parts of the problem.
Some methods help with stuck memories. Some help with body-based survival responses. Others help you understand the protective parts of your personality that formed around pain.
What each approach tends to do best
Somatic approaches focus on the body’s stress responses. These methods help clients notice activation, discharge survival energy gradually, and build tolerance for emotions without overwhelm. They are especially helpful when someone says, “I know what happened, but my body still reacts.”
EMDR can be useful when specific memories, emotional flashbacks, or recurring relational triggers feel frozen in time. It helps people process experiences that still carry a strong emotional charge.
Internal Family Systems or parts work helps clients relate differently to the parts that cling, numb out, criticize, please, or avoid. Instead of fighting those parts, therapy gets curious about what they protect.
Attachment-focused relational therapy uses the therapeutic relationship itself as part of treatment, an essential aspect because attachment wounds formed in relationship and often need relational repair, not just private insight.
Why integration usually works better than purity
Clients sometimes ask which modality is best. That is usually the wrong question.
The better question is whether the therapist can match the method to your nervous system, your history, and your current capacity. A highly structured protocol may help one person feel held and overwhelm another. Open-ended exploration may help one person deepen and leave another drifting.
A grounded attachment trauma therapist often moves flexibly. They may use regulation tools when you are flooded, parts work when you are conflicted, and memory processing when your system has enough safety.
Research supports relational approaches
One of the clearest examples comes from Attachment-Based Family Therapy. A landmark randomized controlled trial described in this PMC review of ABFT outcomes found that after 16 weeks, 87% of participants no longer met criteria for major depressive disorder, with significant reductions in suicidal ideation. That is a strong reminder that repairing relational ruptures can produce meaningful clinical change.
One option among many
For adults seeking this kind of work, practices vary widely. Some clinicians specialize in EMDR. Some emphasize somatic work. Some combine attachment, trauma-informed counselling, and nervous system regulation in an online format. Securely Loved is one example of an attachment-focused practice that offers therapy and learning resources for adults working through anxious, avoidant, or disorganized patterns.
The right fit is usually the therapist whose approach helps you feel both safe and gently challenged.
Navigating Midlife and Hormonal Changes with Support
Many adults are startled when old attachment patterns intensify in midlife. They thought they had outgrown the anxiety, the shutdown, or the fear of being left. Then a breakup, divorce, caregiving strain, empty nest transition, or hormonal shift hits, and everything feels closer to the surface.
That does not mean you are failing. It often means your system has less spare capacity than it once did.

Why old wounds can feel new again
During midlife, many people juggle multiple forms of change at once. Relationships shift. The body changes. Roles change. Loss becomes less abstract.
When hormones fluctuate, the nervous system can feel more sensitive and less buffered. Reactions that used to feel manageable may suddenly feel sharp, immediate, or exhausting. A text delay hits harder. A conflict lingers longer. Sleep disruption lowers resilience even further.
This is one reason embodied attachment work matters so much in this season. You are not just changing thoughts. You are supporting a system under more strain.
For readers navigating this overlap, this resource on menopause and anxiety symptoms may help connect the dots.
Life transitions increase relapse risk
Some transitions reopen attachment wounds even after good therapy. One source notes that up to 55% of adults can revert to insecure attachment patterns within 18 months after therapy if they face a major relational trigger such as a breakup or divorce, according to this discussion of attachment relapse during trauma recovery.
Whether or not that exact number fits your experience, the clinical point is important. Healing needs maintenance. A regulated season of life can make progress feel stable. A major rupture can expose where more support is still needed.
What helps during this stage
A midlife attachment approach often works best when it includes both insight and daily regulation.
- Track your state, not just your story. Notice when your body shifts into urgency or collapse.
- Reduce shame about needing support. Increased sensitivity is not weakness.
- Use transition periods intentionally. Breakups, caregiving stress, and hormonal shifts can become openings for deeper repair.
Midlife reframe: If old patterns are resurfacing now, that may be a sign your system is ready for a level of healing that earlier coping strategies kept out of view.
How to Choose the Right Attachment Trauma Therapist
Not every therapist who understands anxiety or relationships is trained to work with attachment trauma. That difference matters.
A therapist can be warm and well-meaning and still move too fast, stay too cognitive, or miss what your nervous system is communicating.
Questions worth asking on a consultation call
Try listening for how the therapist thinks, not just how they market themselves.
- How do you work with the body and nervous system in session?
- What do you do when a client becomes overwhelmed or shuts down?
- How do you understand co-regulation and relational safety?
- How do you pace trauma work with clients who have attachment wounds?
- Do you use approaches like parts work, somatic tools, EMDR, or attachment-focused interventions?
Their answers should sound specific and grounded. You want more than “I provide a safe space.”
Green flags and red flags
A useful way to decide is to notice what the therapist centers.
| Green flags | Red flags |
|---|---|
| Talks about pacing and consent | Pushes for disclosure too quickly |
| Understands shutdown, panic, and avoidance as protective | Labels you as resistant or difficult |
| Includes body awareness and regulation | Focuses only on changing thoughts |
| Welcomes feedback and repair | Gets defensive or rigid |
| Understands relational dynamics in midlife and transitions | Treats symptoms in isolation |
Fit matters more than impressive language
Some people choose therapists based on credentials alone. Credentials matter, but fit is lived, not abstract.
Do you feel rushed? Do you feel subtly judged? Does the therapist seem comfortable with complexity, or do they force your experience into a simple script?
A good attachment trauma therapist does not try to overpower your defenses. They understand that your defenses were built for reasons. They help you become safer inside yourself so those protections can soften over time.
If a consultation leaves you feeling pressured, confused, or emotionally flooded, listen to that. You do not need a therapist who performs expertise. You need one who can help your system experience safety, clarity, and honest repair.
Your Next Step Toward Secure Connection
Attachment trauma therapy helps you do something profound. It helps you stop treating your survival pattern like your personality.
The anxiety, distancing, overgiving, shutdown, or push-pull dynamic you keep repeating is not random. It is learned. And what is learned in relationship can be healed in relationship, with the right pace and support.
Secure connection does not mean you never get triggered again. It means you recognize what is happening sooner. You recover faster. You ask for what you need more clearly. You choose from self-trust instead of old fear.
If you are tired of understanding your pattern but still feeling trapped inside it, this work can help. If midlife changes, heartbreak, or emotional overwhelm have made everything feel raw again, this work can help. If years of traditional talk therapy gave you insight but not enough change, attachment trauma therapy may be the missing piece.
Healing starts with one grounded next step, not a grand leap.
If you want support with attachment wounds, nervous system regulation, and repeating relationship patterns, you can book a free 15-minute connection call with Securely Loved. It is a private, no-obligation space to talk about what is happening, what you want to change, and whether the fit feels right.
