
Navigating Perimenopause Anxiety and Depression
Some women arrive in my practice saying, “I don’t recognize myself anymore.” They’re still competent. They’re still showing up for work, family, and everyone else. But inside, something feels badly off. Their patience is gone. Their sleep is unreliable. Their chest feels tight for no obvious reason. They cry over things that wouldn’t have touched them a year ago, or they feel strangely flat and disconnected.
Just as often, they assume the problem is personal. They think they’re becoming too needy, too angry, too sensitive, too much. If they already carry anxious or disorganized attachment patterns, perimenopause can intensify every old fear. A delayed text suddenly feels devastating. A hard conversation with a partner feels like proof the relationship is failing. A normal work stressor feels impossible to tolerate.
Understanding perimenopause anxiety and depression changes everything. It doesn’t erase the pain, but it gives the pain a context. And that context matters. When you understand what hormones are doing to your brain and nervous system, and how attachment history can shape the way you interpret those sensations, you stop treating yourself like the problem. You start responding with precision, compassion, and the right kind of support.
You're Not Losing Your Mind It Might Be Perimenopause
One of the most common stories I hear goes like this. A woman who has always been capable and emotionally insightful starts feeling hijacked by her own reactions. She wakes at 3 a.m. with dread. She snaps at her partner, then feels ashamed. She forgets simple things, feels foggy in meetings, and starts wondering whether she’s depressed, burnt out, or falling apart.
That experience is frightening. It’s also far more recognized than many women realize.

What this can look like in real life
You might still be functioning on the outside while feeling completely unlike yourself on the inside. That mismatch often creates extra shame because other people can’t see the inner chaos.
A few examples I see with clients:
- At work you prepare for a meeting you’ve handled many times before, but your body floods with dread anyway.
- At home your partner asks a simple question and you hear criticism, pressure, or rejection.
- In your own mind you keep searching for a reason you feel so bad, and if you can’t find one, you decide it must be you.
When familiar coping strategies stop working, many women assume they’ve become emotionally weaker. Often, their hormones and nervous system are simply under strain in a new way.
Perimenopause can show up through mood swings, brain fog, irritability, anxiety, sadness, rage, or a sense that your emotional volume knob is stuck too high. If your cycle has become less predictable, your sleep has worsened, or your body suddenly feels less resilient, that context matters.
For a practical overview of cycle changes and what they can mean, this expert guidance on perimenopause for women offers a useful starting point.
The relief of naming it
Once women can say, “This may be perimenopause,” the self-blame often softens. Not disappears. Softens.
That’s an important turning point, because you can’t respond well to something you keep mislabeling. If you call a hormonal and nervous system shift a character flaw, you’ll choose the wrong solutions. If you recognize it for what it is, you can start getting traction.
Why Your Hormones Can Hijack Your Mood
Perimenopause often feels confusing because the mood changes can seem to come out of nowhere. They don’t. They come from a body that’s trying to adapt to hormonal fluctuation.
I often explain it like this. Your brain and hormones are supposed to work like an orchestra with a conductor. During perimenopause, the conductor keeps dropping the baton. The instruments are still there, but timing, coordination, and tone become less predictable. That’s why your emotional state can feel so inconsistent from one day to the next.
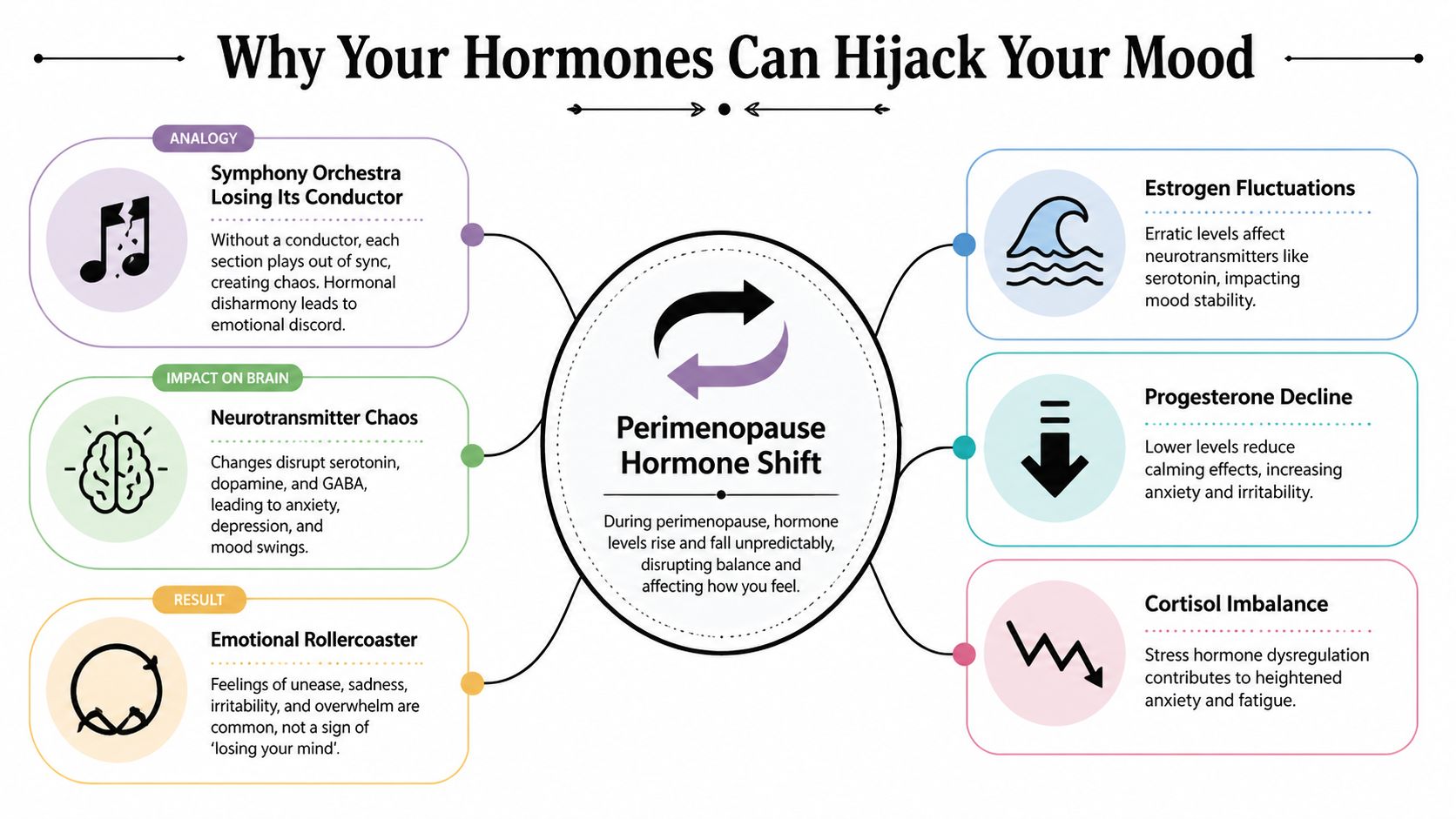
Estrogen, progesterone, and stress chemistry
Estrogen helps support brain systems involved in mood regulation, including serotonin. When estrogen becomes erratic, some women feel more tearful, flattened, irritable, or emotionally fragile.
Progesterone is often experienced as more calming. When it declines or fluctuates unpredictably, sleep can worsen and the nervous system can feel less buffered. That can mean more agitation, more internal buzzing, and less capacity to recover after stress.
Then there’s cortisol, your stress hormone. When sleep is poor, hot flashes are disruptive, and hormones are swinging, cortisol regulation can get messy. Your body may start acting as if it’s under threat even when your life circumstances haven’t changed much.
Why this matters clinically
Perimenopause is not just a physical transition. It is also a mental health vulnerability window. Perimenopause markedly increases the risk of depression and anxiety, with a 2 to 5 times higher incidence of major depressive disorder compared to premenopausal or postmenopausal stages. A 2024 meta-analysis reported a 34% prevalence of depression in perimenopausal women worldwide, while anxiety affects over 50%, according to this perimenopause depression and anxiety treatment guide.
That doesn’t mean every woman will develop a disorder. It does mean your emotional symptoms deserve to be taken seriously.
Clinical reality: if your mood changed sharply during hormonal transition, “just push through” is usually poor advice.
What hormonal mood disruption tends to feel like
The emotional impact is often broader than simple sadness or worry. Women describe:
- A shorter fuse with children, partners, colleagues, or noise
- A dread response that appears before ordinary tasks
- Nighttime spiraling when sleep disruption and anxiety feed each other
- A loss of emotional predictability, which can feel especially scary if you’re used to being steady
Hormonal shifts also affect the brain indirectly. If you’re sleeping badly, overheating at night, or feeling physically uncomfortable, your resilience drops. Small stressors hit harder. You recover more slowly. What would once have been annoying now feels overwhelming.
For a fuller explanation of how these shifts can present, I recommend reading about menopause and anxiety symptoms.
What doesn’t work well
Trying to reason your way out of a hormonally activated nervous system rarely works in the moment. So does shaming yourself for being reactive. So does assuming every intense feeling is a sign that your marriage, career, or identity is collapsing.
Those interpretations can come later if needed. First, stabilize the body that’s sounding the alarm.
Untangling Your Perimenopause Symptoms
Many women ask me a version of the same question. “How do I know if this is hormones, depression, anxiety, or something deeper?”
The honest answer is that there can be real overlap. But the pattern still matters. The timing matters. The body context matters.
Symptom patterns matter more than self-judgment
One useful finding is that perimenopausal women don’t all experience this transition in the same way. In one analysis, 56.5% were in a low-symptom group, 33.7% had borderline depression-anxiety symptoms, and 9.8% experienced severe comorbidity. Key risk factors included a history of mental illness, sleep disorders, and severe physical perimenopausal symptoms, as reported in this analysis of symptom profiles in perimenopausal women.
That matters because many women dismiss themselves by saying, “Other people seem fine, so maybe I’m just not coping well.” But symptom burden varies. It is not a moral test.
How hormonally driven symptoms often feel
Perimenopause-related mood shifts often have a distinct texture. They may feel sudden, disproportionate, physically charged, and less connected to a clear story.
Here’s a practical way to consider it:
| Experience | More suggestive of hormonal influence | More suggestive of long-standing pattern |
|---|---|---|
| Anxiety | Sudden surges, body-based dread, often worse with sleep disruption or cycle changes | More consistent themes and familiar triggers over time |
| Low mood | Flatness, irritability, tearfulness, “I don’t feel like myself” | A more recognizable depressive pattern from earlier life |
| Relationship distress | Reactions intensify quickly, especially when exhausted or flooded | Repeating relational fears that predate this life stage |
| Cognitive symptoms | Brain fog, word-finding issues, forgetfulness during hormonal instability | Concentration issues tied more clearly to chronic stress or depression |
This isn’t a diagnostic tool. It’s a way to become more observant and less self-attacking.
Common presentations I see
Some women don’t look “depressed” in the commonly imagined stereotype. They look irritable, impatient, numb, or intensely anxious.
Common forms include:
- Rage and irritability that seem to arrive faster than your usual coping can catch
- Flat-lining depression, where motivation drops and everything feels gray rather than dramatic
- Panic-like episodes that feel physical first and mental second
- Social fragility, where normal interactions suddenly feel exposing or exhausting
A symptom doesn’t have to look neat to deserve care. Perimenopause often blurs the line between emotional, physical, relational, and cognitive distress.
If you want a broader checklist of body and mood changes, this guide to perimenopause symptoms and treatment can help you notice patterns you may have missed.
Questions worth tracking
Bring these into a journal or a medical appointment:
- When did the mood change start?
- What’s happening with sleep, cycle changes, hot flashes, or night sweats?
- Do symptoms surge at certain times of the month?
- What feels new, and what feels familiar from earlier periods of stress?
That kind of tracking helps you stop arguing with yourself and start gathering usable information.
How Your Attachment Style Shapes Your Perimenopause Experience
Perimenopause doesn’t happen in a psychological vacuum. It lands in a nervous system with a history.
That’s where attachment matters. The hormonal upheaval of this stage can feel destabilizing for anyone. But if you grew up with inconsistent emotional attunement, criticism, unpredictability, or emotional neglect, your system may already be primed to read internal discomfort as danger.

Why old attachment wounds get louder now
I see this with my clients all the time. A woman enters perimenopause and suddenly her usual emotional coping doesn’t work. Her body feels more reactive. Her sleep is thinner. Her tolerance for ambiguity collapses.
If she has an anxious attachment pattern, she may start scanning constantly for signs that something is wrong in her relationship. If she has an avoidant attachment pattern, she may pull away further because the internal intensity feels unbearable. If she has a disorganized attachment pattern, she may swing between reaching for reassurance and wanting to disappear.
The biology is real. So is the attachment lens interpreting it.
The perfect storm effect
The connection between attachment and hormonal vulnerability is not theoretical. Women with a prior history of depression face a 58% greater risk for a depressive episode during perimenopause, and the attachment-hormone link is discussed in this menopause and mental health resource. For women whose earlier life experiences already shaped a hypervigilant nervous system, perimenopause can create a kind of perfect storm.
That doesn’t mean your childhood “caused” your hormones. It means your history influences how your body and mind process the instability.
A hormonally activated body can feel like abandonment, danger, shame, or impending loss when old attachment wounds are close to the surface.
What this looks like in relationships
A secure nervous system usually has more room to say, “I’m overwhelmed today. Let me slow down and come back to this.” An insecurely attached nervous system is more likely to jump to interpretation.
Here’s how that can play out:
Anxious attachment
- Your partner seems distracted.
- You feel a spike of panic.
- The story becomes, “They don’t care anymore.”
Avoidant attachment
- You feel emotionally flooded and ashamed of needing support.
- The story becomes, “I need to handle this alone.”
Disorganized attachment
- You want comfort and fear it at the same time.
- The story becomes, “I’m too much, but please don’t leave.”
Those reactions are painful, but they’re also understandable. If your system learned early that connection was inconsistent, then perimenopausal instability can amplify every unresolved alarm.
If you’re not sure how to name your own pattern, this explanation of attachment style definitions can help you make sense of what’s happening.
What does help
The women who tend to find the most lasting relief don’t only ask, “Which hormone is changing?” They also ask, “What old fear does this sensation wake up in me?”
That question changes treatment. It shifts the goal from suppressing symptoms to understanding them. It also helps you stop making major relationship conclusions in the middle of a hormonally and attachment-driven storm.
Finding What Works Medical and Therapeutic Treatments
When perimenopause anxiety and depression hit hard, women are often offered an unhelpful false choice. Either it’s “just hormones” and you should see a medical provider, or it’s “just emotional” and you should go to therapy.
In practice, that split usually fails people. The best care often addresses both.
Medical treatment and what it can help with
There are times when a medical intervention is not only appropriate, but relieving. If hormone fluctuation is a major driver, hormone therapy may help stabilize some of the volatility for women who are appropriate candidates. If depression or anxiety symptoms are more entrenched, SSRIs or SNRIs may be part of the picture. Some women also need direct treatment for sleep disruption because poor sleep can make everything else harder to treat.
This isn’t about ideology. It’s about fit.
A useful question to bring to a clinician is not “Should I be natural or medical?” It’s “Which symptom cluster is driving the most impairment right now?”
For broader reading on nonprescription strategies and lifestyle supports, The Axelrad Clinic's guide on perimenopause offers a grounded overview.
Therapy and where it can miss the mark
Traditional talk therapy can be helpful, but it often falls short when it stays only at the level of insight. Many women already understand why they feel bad. What they don’t yet know is how to calm a body that keeps sounding the alarm.
When therapy doesn’t account for the nervous system, clients can leave sessions with excellent intellectual understanding and no more ability to regulate in real life. That’s especially true when attachment trauma is involved.
A clearer comparison
| Support type | Best use | Limitation if used alone |
|---|---|---|
| Hormone-focused care | Useful when mood shifts track strongly with hormonal change, vasomotor symptoms, or sleep disruption | Doesn’t resolve attachment fears, shame, or relational patterns |
| Medication for mood or anxiety | Useful when symptoms are persistent, severe, or impairing daily function | May reduce intensity without changing how you interpret distress |
| Talk therapy | Helpful for meaning-making, grief, stress, and relationship reflection | Can stay too cognitive if the body remains dysregulated |
| Trauma-informed and somatic work | Helps build internal safety and reduce hypervigilance | May need medical support alongside it if hormonal symptoms are intense |
Why integrated care matters
The urgency here is not small. The global burden of anxiety disorders in perimenopausal women is projected to surge by 40.67% by 2035, according to this global analysis of anxiety burden in perimenopausal women.
Women need treatment pathways that reflect reality. Hormonal symptoms are real. Psychosocial stress is real. Attachment wounds are real. Sleep disruption is real. Trying to treat only one layer often leads to partial relief and ongoing confusion.
What works best: the body gets support, the nervous system gets regulation, and the emotional history gets care.
What I’d encourage you to ask
When you meet with a clinician or therapist, ask questions that reveal whether they can think in an integrated way:
- Do they understand menopause-related mood shifts?
- Do they ask about sleep, cycle changes, and vasomotor symptoms?
- Do they explore trauma history and attachment patterns without reducing everything to childhood?
- Do they offer practical regulation tools, not just insight?
If the answer is no across the board, it may not be the right fit.
Everyday Tools for Nervous System Regulation
When your system is flooded, the first job is not to solve your whole life. It’s to reduce the sense of internal danger.
Many women interpret perimenopausal nervous system activation as proof that they’re failing, losing control, or in the wrong relationship. That interpretation spiral can make symptoms worse. The psychological interpretation crisis is a real treatment target, and this Stanford discussion of mental health in menopause and perimenopause speaks to how women can misread hormonally driven distress.

Four tools that help in the moment
These aren’t glamorous. They are effective because they give your body a different signal.
Box breathing
Inhale for a count of four. Hold for four. Exhale for four. Hold for four. Repeat a few rounds without forcing it.
Why it helps: the structure interrupts spiraling and gives your nervous system a rhythm to follow. If counting makes you more tense, shorten the count and focus on a longer exhale.
Orienting
Turn your head slowly and let your eyes land on a few neutral or pleasant objects in the room. Name them in your mind. Notice color, shape, and distance.
Why it helps: anxious states narrow attention around threat. Orienting reminds your body that you are here, in this room, in this moment.
Bilateral tapping
Cross your arms over your chest or tap one hand on each thigh, alternating left and right. Keep the rhythm steady and gentle.
Why it helps: alternating stimulation can reduce overwhelm and help organize a scattered internal state.
Temperature and texture grounding
Hold a cool glass, touch a smooth stone, run your hands under warm water, or wrap up in a textured blanket.
Why it helps: sensory input can pull you out of mental spiraling and back into the body in a manageable way.
A simple practice sequence
If you’re not sure where to begin, use this order:
- Pause the story. Don’t decide what the feeling means yet.
- Name the state. “I’m flooded.” “I’m activated.” “My body feels unsafe right now.”
- Use one body-based tool for a few minutes.
- Reassess before acting, texting, arguing, quitting, or making a major decision.
You don’t need to trust your first interpretation when your nervous system is in alarm.
A fuller set of practical supports is available in these ways to regulate your nervous system.
Guided support can help you practice
Sometimes it’s easier to regulate with someone guiding the pace. This video offers a supportive place to start with a calming exercise from Bev Mitelman’s channel:
What people often do that backfires
A few habits commonly make perimenopausal anxiety worse:
- Over-explaining while flooded instead of regulating first
- Doom-scrolling symptoms late at night when the body is already activated
- Interrogating the relationship during a hormonal crash
- Treating every feeling as a fact
These tools won’t fix everything. They do create enough internal safety to stop the cascade.
When to Seek Help and Your Path to Healing
Self-help tools are useful. They are not always enough.
If your anxiety or depression is interfering with work, sleep, relationships, or your ability to care for yourself, it’s time to seek more support. The same is true if your moods feel frighteningly intense, if you’re experiencing panic, if your relationship is taking repeated hits because of emotional flooding, or if you can’t tell what’s hormonal and what’s trauma-related anymore.
Signs it’s time to reach out
Please seek professional support if any of the following are true:
- You’re having thoughts of self-harm or hopelessness
- You can’t function reliably in daily life
- Your sleep disruption is persistent and worsening your mental health
- You’re making major relationship or life decisions from a chronically dysregulated state
- You’ve tried standard talk therapy and still feel stuck in the same fear loops
You do not need to wait until things are unbearable.
Healing is more possible when the full picture is addressed
The women who begin to feel more like themselves usually stop asking one narrow question. They stop asking only, “What’s wrong with me?” and start asking better ones.
Questions like:
- What is my body trying to signal right now?
- What part of this is hormonal?
- What part of this is old attachment pain getting activated?
- What support would help me feel safer, steadier, and less alone?
I see this shift with my clients. Relief often starts when they realize they are not crazy, not weak, and not failing at adulthood. They are moving through a real hormonal transition in a nervous system shaped by lived experience.
Seeking help during perimenopause is not overreacting. It is a wise response to a complex transition.
What to look for in support
Good support should help you do three things at once:
| Need | Helpful support |
|---|---|
| Clarify symptoms | A provider who understands menopause-related mood changes |
| Reduce suffering | Treatment for sleep, anxiety, depression, or hormonal instability when needed |
| Create lasting change | Therapy that addresses attachment patterns, regulation, and relational safety |
If you can find care that respects both your biology and your biography, you’re much more likely to feel grounded again.
Healing during perimenopause usually isn’t about one perfect solution. It’s about the right combination. Medical care when appropriate. Therapy that goes deeper than insight. Practical regulation tools that work in real life. Self-compassion strong enough to replace shame.
If this article felt uncomfortably familiar, Securely Loved offers a compassionate next step. Bev Mitelman supports adults navigating attachment wounds, emotional overwhelm, relationship anxiety, and midlife hormonal transitions through trauma-informed, attachment-focused care. You can book a free 15-minute connection call to explore fit in a private, no-pressure space. If you’re not ready for therapy yet, the site also offers an attachment style quiz, courses, and practical resources to help you understand your patterns, regulate your nervous system, and move toward a more secure relationship with yourself and others.
