
What Is Somatic Therapy For Trauma: A Guide
You know the moment. A text comes in from your partner that says, “Can we talk later?” Your mind tells you this could mean anything. Your body acts like danger has already arrived. Your chest tightens. Your stomach drops. You start rehearsing what you did wrong, or you go cold and stop feeling much of anything at all.
That split is often what brings people to ask, what is somatic therapy for trauma. You may understand your patterns. You may already know your childhood shaped your attachment style. You may have spent years in therapy naming your triggers with impressive clarity. Yet the body still reacts first.
That doesn’t mean you’ve failed at healing. It usually means the part of you carrying the alarm isn’t your thinking mind. It’s your nervous system.
Somatic therapy works with that reality. Instead of asking you to explain yourself better, it helps you notice what your body is doing in real time and gently shift the pattern from the inside out. For some people, this becomes an important complement to comprehensive PTSD treatment when trauma symptoms show up both emotionally and physically.
This approach is also gaining attention far beyond niche trauma circles. One market analysis projects the global somatic therapy market will grow from USD 4.83 billion in 2025 to USD 24.85 billion by 2035, with a 17.8% CAGR, while noting that more than 60% of adults report experiencing at least one traumatic event (somatic therapy market analysis). People are looking for something deeper than coping. They’re looking for relief that their body can feel.
When Your Body Remembers What Your Mind Wants to Forget
You can know you’re safe and still not feel safe.
That’s common in trauma, especially attachment trauma. A raised voice, delayed reply, emotional distance, or even someone being kind to you can trigger a body response that feels far bigger than the moment itself. Your nervous system may react as if an old threat is happening again.
Why this happens in relationships
Relationships activate the deepest learning your body holds about safety, closeness, and abandonment. If love once felt inconsistent, intrusive, rejecting, or unpredictable, your body may still brace for those outcomes. You may call this anxiety, overthinking, numbing, or self-sabotage. Somatic therapy sees the pattern underneath.
A useful starting point is learning what regulation feels like in your body. This guide on nervous system regulation can help you recognize the difference between true safety and temporary shutdown.
You don't need more self-criticism when your body is protecting you with an old strategy.
What somatic therapy does differently
Somatic therapy doesn’t start by pulling apart every detail of the past. It often starts with a simple question: what are you noticing right now?
That might be heat in your face, pressure in your throat, fluttering in your chest, tension in your jaw, or a foggy blankness that tells you you’ve gone offline. These sensations aren’t random. They are clues.
In practice, somatic work helps you:
- Notice activation earlier so you don’t only realize you’re triggered after a spiral, shutdown, or conflict
- Stay with small pieces of sensation rather than getting swallowed by the whole story
- Build capacity for safety so closeness, rest, and vulnerability stop feeling so threatening
- Change relational reflexes that keep repeating even when you “know better”
If talk therapy gave you insight but not enough change, this is often the missing layer. Healing starts to stick when your body no longer has to carry the past alone.
The Science of a Traumatized Nervous System
A traumatized nervous system works like a smoke alarm that kept blaring after the fire ended.
The original danger may be long over. But the alarm still goes off when there’s steam from the shower, toast in the oven, or someone moving too fast in the kitchen. That isn’t because the alarm is stupid. It’s because it learned that missing danger felt too costly.
Trauma can affect the brain in a way that makes this even more understandable. Somatic Experiencing uses a bottom-up model because trauma can cause the prefrontal cortex to go offline, which is why logic often disappears in the moments you need it most. Rather than relying on cognitive narrative, it works with interoceptive sensations so the nervous system can complete interrupted survival responses and experience something different from helplessness (research overview on Somatic Experiencing).
A broader look at therapy for emotional well-being can also help if you're trying to understand how physical symptoms and emotional distress reinforce each other.
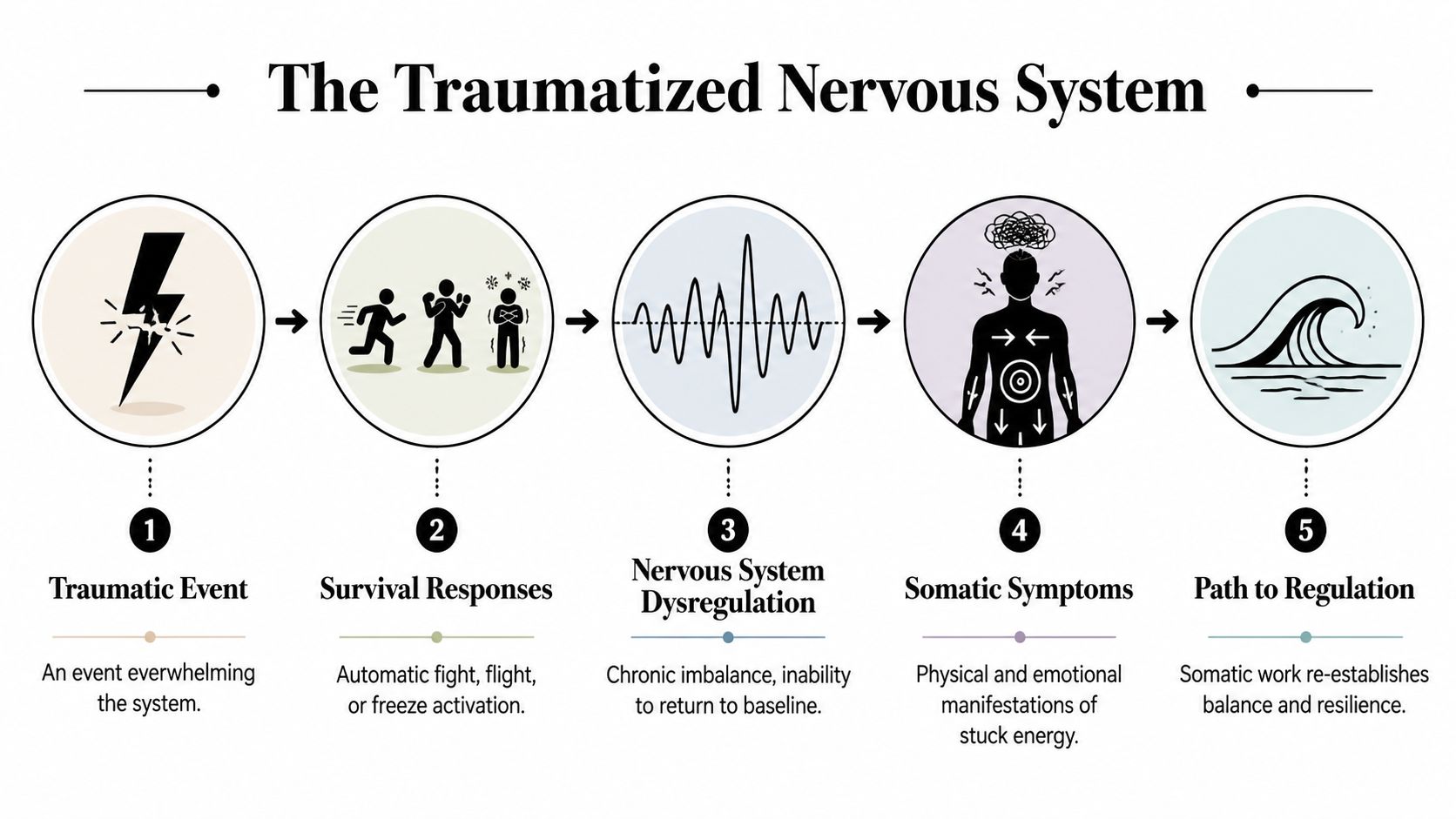
Your nervous system has protective gears
If you’ve been reading about trauma, you may have heard terms from Polyvagal Theory. You don’t need to memorize them. It helps more to understand them as body states.
Here’s a simple way to think about them:
| State | What it feels like | How it often shows up in relationships |
|---|---|---|
| Calm and connected | Open, grounded, able to think and feel at once | You can stay present during conflict and repair |
| Fight or flight | Fast, tense, activated, scanning | You over-explain, protest, chase, panic, argue, obsess |
| Freeze or shutdown | Heavy, numb, foggy, collapsed | You pull away, go blank, disconnect, say “I’m fine” |
When your alarm system gets stuck in high alert, your body starts reading ordinary stress like a fresh emergency. That’s often what people mean when they talk about nervous system dysregulation. Your system struggles to return to baseline after activation.
Why thinking alone often doesn't work
When someone says, “Just calm down,” it usually doesn’t help because the body isn’t asking for advice. It’s running a survival program.
You might know:
- your partner is late because work ran over
- your boss’s short email doesn’t mean you’re in trouble
- your friend taking space doesn’t automatically mean rejection
But if your nervous system links uncertainty with danger, your body reacts before your beliefs can catch up.
Practical rule: If your body is in survival mode, insight is helpful but incomplete.
What bottom-up healing looks like
Bottom-up therapy starts with the body and lets meaning emerge from there. You might notice your shoulders lift when you talk about setting a boundary. You might realize your breath disappears when someone gets emotionally close. You might feel a rush in your legs when you remember a time you couldn’t leave.
The point isn’t to perform your trauma or relive it in full detail. The point is to help your system complete what got interrupted.
That often includes:
- tracking sensations instead of forcing a polished explanation
- slowing down when the body speeds up or goes numb
- building choice between trigger and reaction
- practicing return to steadiness after activation
The smoke alarm metaphor matters here. Somatic work doesn’t rip the alarm out of the ceiling. It helps recalibrate it, so it can respond to real danger without treating every signal as a fire.
Core Techniques That Help the Body Heal
The words can sound abstract until you see how they work in real life. In session, somatic techniques are usually quiet, gradual, and far less dramatic than people expect.

Titration helps you approach without flooding
A client starts describing a fight with her partner. Within seconds, her chest tightens and her hands go cold. In older therapy experiences, she would keep talking while getting more overwhelmed, then leave session exhausted and raw.
With titration, we don’t dive deeper just because the story is important. We slow down and take one small piece. Maybe we stay only with the chest tightness for a few moments. Maybe we notice what happens when she says the single phrase, “I felt dismissed,” and stop there.
Before, her body experienced therapy as another overwhelm.
After practicing titration, she starts to feel, “I can touch this without drowning in it.”
Pendulation teaches movement, not stuckness
Another client comes in after being ignored for several days by someone he’s dating. His whole system is activated. He wants to analyze every text, every pause, every possible reason.
With pendulation, we move gently between activation and something steadier. He notices the agitation in his chest. Then he looks around the room, feels the support of the chair, and notices that his feet are warm. Then we return briefly to the activation. Then back again.
This back and forth matters. Trauma gets the body stuck in one state. Pendulation teaches, “I can move. I’m not trapped here.”
Sometimes healing is not about going deeper into pain. It’s about learning you can come back out.
Resourcing gives your body somewhere to land
A woman with avoidant attachment tells me she feels “nothing” whenever someone wants more closeness. If we push into sensation too fast, she leaves herself. So we begin with resourcing.
That might be:
- an external resource like a blanket, a window view, or the feeling of her feet inside steady shoes
- an internal resource like the sensation of strength in her back
- a relational resource like remembering one moment of being understood without pressure
Before resourcing, closeness feels invasive and body awareness feels unsafe.
After resourcing becomes familiar, she has a place to return to when vulnerability stirs alarm.
If you want simple practices you can use between sessions, these grounding techniques for trauma are a good starting point.
What these techniques do together
Titration says, “small enough to stay present.”
Pendulation says, “you can move between discomfort and ease.”
Resourcing says, “you don’t have to do hard things without support.”
That combination is part of why somatic work often fits people who’ve tried insight-focused therapy and still feel hijacked by their bodies. It can also pair well with other trauma treatments. For example, some people exploring EMDR therapy for relapse triggers are also looking for body-based ways to manage activation before and after deeper processing work.
Somatic Therapy vs Traditional Talk Therapy
Talk therapy and somatic therapy are not enemies. They answer different parts of the same problem.
If you’ve said, “I understand why I do this, but I still do it,” you’re naming the gap between insight and embodied change. That gap matters most in trauma and attachment work.
The first randomized controlled trial on Somatic Experiencing found that people with PTSD who received 15 weeks of treatment showed substantial improvements in post-traumatic symptoms and depression, with Cohen’s d ranging from 0.7 to 1.26, supporting its clinical effectiveness (randomized controlled trial on Somatic Experiencing).
Comparing top-down and bottom-up healing
| Aspect | Traditional Talk Therapy (Top-Down) | Somatic Therapy (Bottom-Up) |
|---|---|---|
| Primary focus | Thoughts, beliefs, emotions, narrative | Sensations, activation, impulses, regulation |
| Starting question | “What happened?” or “What were you thinking?” | “What do you notice in your body right now?” |
| Role of the past | Builds a coherent story and meaning | Tracks the physiological imprint that remains |
| Main tool | Reflection, interpretation, cognitive insight | Sensation tracking, pacing, grounding, body awareness |
| Common marker of progress | Better understanding and language | More regulation, less reactivity, more choice |
| Best use case | Patterns you can think through and integrate verbally | Patterns that keep firing even when you understand them |
Where each one shines
Talk therapy can be valuable when you need language, perspective, grief processing, relational context, or help challenging distorted beliefs. Many people need that. Many people benefit from both.
Somatic therapy becomes especially important when:
- your body overrides your logic
- you shut down before you can speak
- you get flooded in conflict
- you know your attachment style but can’t interrupt it live
What doesn't work well
What usually doesn’t help is trying to force one method to do the whole job.
If you only analyze but never work with the body, you may become highly insightful and still feel chronically unsafe. If you only focus on sensation without context, you may miss meaning, boundaries, and patterns in relationships.
Good trauma therapy doesn't ask you to choose between understanding and regulation. It helps both happen.
For many clients, somatic work is not a replacement for talk therapy. It’s the layer that finally helps insight take root.
How Somatic Work Heals Anxious and Avoidant Attachment
The question what is somatic therapy for trauma often takes on a personal dimension. Those asking it aren’t only trying to heal one frightening event. They’re trying to stop repeating painful relationship patterns that make no sense on paper but feel automatic in the body.
A real gap exists here. There is minimal explicit guidance in the clinical literature on how techniques like titration and pendulation specifically resolve attachment-driven relationship patterns. That gap matters because it points to a practical need: showing how somatic work can shift the nervous system’s relational “set point” for people with anxious or avoidant styles who haven’t found enough relief through insight-focused approaches (discussion of the attachment gap in somatic therapy).

Anxious attachment often lives in a body that can't settle
If you have anxious attachment, your system may move quickly into pursuit. You text again. You replay the conversation. You search for reassurance. You tell yourself you’re “too much,” but the deeper truth is often that your nervous system has linked distance with danger.
Somatic work helps by interrupting the physical escalation before it becomes relational panic.
That can look like:
- noticing the first rush in your chest before you send the fifth text
- feeling your feet on the floor while the urge to chase rises
- naming, “my body is bracing for abandonment,” instead of treating the sensation as proof
- practicing regulation before contact, not only after a rupture
The goal isn’t to become detached. It’s to help your body tolerate uncertainty without collapsing into alarm.
Avoidant attachment often protects through shutdown
Avoidant patterns can look calm from the outside. Inside, the body may be working hard to reduce overwhelm by muting need, emotion, and contact.
When closeness increases, you may feel tired, foggy, irritated, or suddenly sure the relationship is wrong. That doesn’t always mean the relationship is wrong. Sometimes it means your nervous system has learned that dependence costs too much.
Somatic work doesn’t force emotional intensity. It helps create enough safety for sensation to come online in manageable ways.
A session might focus on:
- the moment your chest goes blank when someone asks what you need
- the impulse to look away or leave when intimacy deepens
- the subtle tension that appears before you detach
- building tolerance for warmth, support, and being seen
For avoidant attachment, progress often looks less dramatic than people expect. It may be staying present two minutes longer. It may be noticing “I want space” without turning that into disappearance.
Disorganized attachment carries both pull and fear
Disorganized attachment often feels like a painful internal split. You want closeness and fear it. You long to be chosen and then distrust care when it arrives. You may swing between pursuit and shutdown so quickly that it feels impossible to track.
Somatic pacing matters most. If therapy moves too quickly, the body can experience even healing as threat. If it moves too slowly without enough clarity, you can stay lost in the pattern.
In good somatic attachment work, the therapist helps you notice the sequence:
- Cue of connection or conflict
- Body activation or collapse
- Protective impulse
- Meaning you automatically assign
- A new regulated choice
That sequence is where change begins. Not because you forced yourself to act secure, but because you learned how your body enters the old loop.
The body often reveals attachment patterns faster than the story does.
Midlife shifts can complicate attachment healing
For many women, hormonal transitions can change the baseline of the nervous system. Tolerance may shrink. Sleep may worsen. Irritability, tears, numbness, or overwhelm may appear faster than before.
That matters in attachment therapy. A response that looks like abandonment panic or avoidant withdrawal may also be intensified by a body under added physiological strain. Good somatic work stays curious about this instead of assuming every reaction means the same thing.
That’s one reason some practitioners work at the intersection of attachment, trauma, and life transitions. Securely Loved offers therapy with that lens, including support for adults healing attachment patterns through nervous system work and midlife transitions. That doesn’t replace medical care when needed, but it can help you sort out what is trauma activation, what is relational patterning, and what may be amplified by a changing body.
What healing looks like in attachment work
Healing doesn’t mean you never get triggered.
It means:
- anxious activation slows sooner
- avoidant shutdown gets easier to notice
- conflict doesn’t erase your sense of self
- closeness stops feeling so dangerous
- you can repair without abandoning yourself
The deepest shift is this. You stop expecting another person to do all the regulating your body never learned how to do alone. That’s when relationships begin to feel less like survival and more like connection.
What to Expect in Your First Somatic Therapy Session
Your first somatic therapy session usually won’t begin with a demand to tell your hardest story.
That surprises many people. If you’ve been bracing for a deep dive into trauma on day one, you can exhale. A good somatic therapist is usually paying close attention to safety, pace, consent, and how your system responds in the moment.
The first question is often about the present
You may hear something like, “What are you noticing in your body right now as you sit here?” That question can feel unfamiliar if you’re used to therapy that begins with history.
You might answer:
- “My chest feels tight.”
- “I’m talking fast.”
- “My hands are cold.”
- “I don’t know what I feel.”
All of those are workable starting points. Even “I don’t know” is useful information. It may mean your system learned long ago that body awareness wasn’t safe.
The therapist is tracking more than your words
A somatic therapist listens to your story, but also watches for cues such as breathing changes, posture shifts, going blank, fidgeting, tension, tears that stop suddenly, or laughter that appears when pain gets close.
That doesn’t mean they are analyzing you in a cold way. It means they are helping you notice patterns that happen faster than language.
A first session may include:
- orientation to the room so your body registers the present environment
- gentle body tracking of sensations without forcing intensity
- resourcing to identify what helps you feel a little steadier
- small pauses if activation rises too quickly
You stay in charge of the pace
One of the most important differences in somatic trauma therapy is that you don’t have to override yourself to “do therapy well.”
You can say:
- “That feels like too much right now.”
- “I’m getting foggy.”
- “Can we slow down?”
- “I need to come back to the present.”
Those are signs of good therapy, not resistance.
A safe first session should leave you feeling more oriented to yourself, not pushed past your limits.
What people often feel afterward
After a first session, some people feel lighter. Some feel tired. Some notice they are more aware of sensations than usual. Some feel relief because no one rushed them.
What matters most is not whether you had a dramatic breakthrough. It’s whether the session helped your body experience even a small increase in safety, clarity, or choice.
You’re not there to prove your pain. You’re there to build a relationship with your nervous system that no longer requires constant emergency management.
Finding a Qualified Somatic Therapist For You
Not every therapist who talks about the body is trained to work with trauma carefully. That distinction matters.
A qualified somatic therapist should understand how to pace activation, recognize shutdown, work with consent, and avoid pushing catharsis for its own sake. Trauma work is not about cracking you open. It’s about helping your system build capacity without overwhelm.
What to look for
Start with basic clinical grounding. Look for a licensed mental health professional or a practitioner with clear trauma training in their scope of practice.
Then look for more specific fit:
- Somatic training: A credential such as Somatic Experiencing Practitioner (SEP) can be a useful sign of specialized training.
- Trauma-informed approach: They should talk about pacing, regulation, and safety. Not just “processing.”
- Attachment knowledge: If your pain mostly shows up in relationships, ask directly how they work with anxious, avoidant, or disorganized patterns.
- Respect for consent: They should be comfortable with slowing down, checking in, and adjusting course.
- Ability to explain their method plainly: If they can’t tell you how sessions work in simple language, that’s a problem.
Green-flag questions to ask
A consultation can tell you a lot. You don’t need to impress the therapist. You’re assessing fit.
Consider asking:
- How do you make sure clients don’t get overwhelmed in session?
- How do you work with shutdown, numbness, or dissociation?
- What experience do you have with attachment trauma and relationship patterns?
- How do you know when to slow down or shift direction?
- What does progress look like in your approach?
Their answers should sound grounded and specific. If they mainly describe intense release, fast breakthroughs, or reliving the past, be careful.
What a good fit feels like
A good fit often feels less flashy than people expect. You may notice that your body doesn’t have to brace as much. You may feel understood without being rushed. You may sense that the therapist can hold complexity without making you perform your pain.
That matters more than perfect wording or a polished website.
If you’re looking for attachment-focused support that includes nervous system work, Securely Loved offers a free 15-minute online connection call where you can ask questions, share what’s been feeling stuck, and see whether the approach fits your needs. The goal isn’t pressure. It’s clarity. When healing has felt confusing for a long time, even one grounded conversation can help you find your next right step.
